We at Crack4sure are committed to giving students who are preparing for the CBIC CIC Exam the most current and reliable questions . To help people study, we've made some of our CBIC Certified Infection Control Exam exam materials available for free to everyone. You can take the Free CIC Practice Test as many times as you want. The answers to the practice questions are given, and each answer is explained.
A patient has an oral temperature of 101° F (38.33 C). Erythema and tenderness arc noted at the central line site. Blood samples are submitted for culture and intravenous vancomycin is ordered. This is an example of which of the following forms of antibiotic treatment?
Empiric
Prophylactic
Experimental
Broad spectrum
Empiric antibiotic therapy is the immediate initiation of antibiotics based on clinical judgment before laboratory confirmation of an infection. In this case, the presence of fever, erythema, and tenderness at the central line site suggests a possible bloodstream infection, prompting empiric treatment with vancomycin.
Step-by-Step Justification:
Initiation Before Lab Confirmation:
Empiric therapy starts treatment based on symptoms while awaiting culture results?.
Prevents Complications:
Delayed treatment in central line-associated bloodstream infections (CLABSI) can lead to sepsis.
Common in High-Risk Situations:
Empiric treatment is used in cases where waiting for lab results could worsen the patient’s condition.
Why Other Options Are Incorrect:
B. Prophylactic:
Prophylactic antibiotics are given to prevent infection, not to treat an existing one.
C. Experimental:
Experimental treatment refers to clinical trials or unproven therapies, which does not apply here.
D. Broad spectrum:
Broad-spectrum antibiotics cover multiple bacteria, but empiric therapy may be narrow-spectrum based on suspected pathogens?.
CBIC Infection Control References:
APIC Text, Chapter on Antimicrobial Stewardship and Empiric Therapy?.
Which of the following is the BEST aid in the identification of patients affected by a recall due to failures in endoscope reprocessing?
Maintaining a log of endoscope use by date of procedure
Maintaining a log of patient identifiers linked with endoscope used
Searching electronic records for endoscope serial number recorded in patient records
Searching electronic records using diagnostic coding to identify all patients that had endoscopy procedures
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes the importance of traceability in endoscope reprocessing programs to ensure rapid and accurate patient notification when reprocessing failures or recalls occur. The most effective method for identifying affected patients is maintaining a log that directly links each endoscope to specific patient identifiers for every procedure.
This type of tracking system allows infection preventionists to quickly determine exactly which patients were exposed to a particular endoscope during the time period of concern. When reprocessing failures are identified—such as incomplete cleaning, high-level disinfection errors, or equipment malfunction—precise linkage between the endoscope and the patient is essential to limit the scope of exposure investigations, reduce unnecessary notifications, and ensure timely follow-up care.
Option A is insufficient because a date-only log does not identify individual patients. Option C may be useful if serial numbers are consistently documented in the medical record, but this practice is not reliably implemented in many facilities and is therefore less dependable. Option D is overly broad and would identify all patients who underwent endoscopy, rather than those exposed to a specific device, leading to unnecessary alarm and inefficient investigations.
For CIC® exam purposes, understanding that patient-to-device linkage logs are the cornerstone of effective exposure investigation and recall management in endoscope reprocessing is critical and aligns with best-practice infection prevention standards.
Catheter associated urinary tract infection (CAUTI) improvement team is working to decrease CAUTIs in the hospital. Which of the following would be a process measure that would help to reduce CAUTI?
CAUTI rate per 1000 catheter days
Standardized Infection Ratio per unit
Rate of bloodstream infections secondary to CAUTI
Staff compliance to proper insertion technique
A process measure assesses how well healthcare personnel follow specific procedures known to prevent infection. In the case of CAUTI (Catheter-Associated Urinary Tract Infection), monitoring staff compliance with proper insertion technique is a direct process measure.
According to the APIC/JCR Workbook, effective CAUTI prevention involves evaluating compliance with proper catheter insertion and maintenance practices. Monitoring this behavior is a process measure that directly affects outcomes like infection rate reduction.
The CBIC Study Guide also emphasizes using compliance with evidence-based insertion techniques as a strategy to measure and improve CAUTI prevention efforts.
APIC Text notes that “a process measure focuses on a process or the steps in a process that leads to a specific outcome.” This includes monitoring healthcare staff performance related to proper catheter insertion and care.
Incorrect answer rationale:
A. CAUTI rate per 1000 catheter days – This is an outcome measure, not a process measure.
B. Standardized Infection Ratio per unit – Also an outcome/benchmarking metric.
C. Rate of bloodstream infections secondary to CAUTI – This is an outcome, not a process.
Passive immunity results from the use of:
Tetanus antitoxin
Hepatitis B vaccine
Influenza vaccine
Human diploid cell rabies vaccine
The Certification Study Guide (6th edition) defines passive immunity as protection that results from the administration of preformed antibodies, rather than stimulation of the individual’s own immune system. Passive immunity provides immediate but temporary protection, because the recipient does not produce antibodies and therefore does not develop immunologic memory.
Tetanus antitoxin is a classic example of passive immunity. It contains antibodies that neutralize tetanus toxin directly and is used in situations where immediate protection is needed, such as after certain wounds in individuals with unknown or inadequate vaccination history. The study guide emphasizes that passive immunization is particularly important in post-exposure management when waiting for an active immune response would be too slow to prevent disease.
The other options represent active immunization, not passive immunity. Vaccines such as hepatitis B vaccine, influenza vaccine, and human diploid cell rabies vaccine stimulate the recipient’s immune system to produce its own antibodies and immune memory. While rabies immune globulin provides passive immunity, the rabies vaccine itself is an active immunizing agent.
This distinction between active and passive immunity is a frequently tested CIC exam concept, especially in the context of occupational health, post-exposure prophylaxis, and immunization programs. Recognizing that passive immunity involves antibody products (antitoxins or immune globulins) rather than vaccines is essential for accurate infection prevention decision-making.
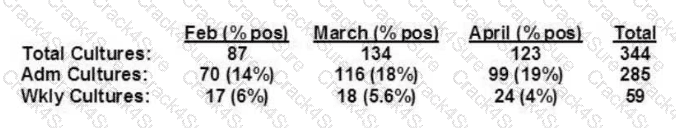
A facility performs active surveillance cultures for methicillin-resistant Staphylococcus aureus (MRSA) on all patients upon admission and weekly. Twenty-two of the patients with positive cultures for MRSA were transferred from outlying facilities. The following MRSA data for a 3-month period are shown. Review of the data reveals which of the following is increasing?
Transmission of MRSA on the unit
Prevalence of MRSA at admission
Patients with MRSA infection
Compliance with collecting MRSA cultures
The table separates admission cultures from weekly cultures, which is a common surveillance approach to distinguish imported MRSA burden (present on admission) from healthcare acquisition (newly detected later). The admission culture percent positive rises over the three months: 14% (Feb) ? 18% (Mar) ? 19% (Apr). That pattern indicates an increasing admission prevalence (option B). NHSN MDRO surveillance methods describe admission prevalence as a proxy measure using admission-related data to quantify organisms present at the time of entry into a location/facility.
By contrast, weekly culture positivity—often used as a proxy for on-unit acquisition/transmission when admission screening is in place—decreases: 6% ? 5.6% ? 4%, so option A is not increasing. The dataset also does not provide information about MRSA infections versus colonization (so C cannot be concluded), nor does it provide a denominator for “compliance” (e.g., expected admissions/weekly screens completed), so D cannot be determined. This interpretation aligns with standard infection prevention use of MRSA surveillance data to track prevalence (burden) versus incidence/acquisition.
Microfiber cloths and mops are preferred over cotton because microfiber:
Is more cost effective.
Is positively charged to better attract dirt.
Can be laundered and dried with other textiles.
Is versatile for both smooth and rough surfaces.
The CBIC Certified Infection Control Exam Study Guide (6th edition) explains that microfiber cleaning materials are preferred over traditional cotton cloths and mops because of their electrostatic properties, which enhance cleaning effectiveness. Microfiber is composed of very fine synthetic fibers that become positively charged, allowing them to attract and trap negatively charged dirt, dust, and microorganisms rather than simply pushing them across surfaces.
This electrostatic attraction enables microfiber to remove a significantly higher percentage of bacteria and organic material from surfaces compared to cotton, even when used with less cleaning solution or disinfectant. The split fiber structure also increases surface area, allowing microorganisms and debris to be captured within the fibers rather than redistributed. These properties make microfiber particularly effective for environmental cleaning in healthcare settings, where surface contamination contributes to transmission of healthcare-associated infections.
Option A is incorrect because microfiber products are often more expensive initially, though they may be cost-effective over time. Option C is incorrect because microfiber must be laundered separately under specific conditions to maintain effectiveness. Option D may be true but is not the primary reason for preference.
For the CIC® exam, it is important to recognize that microfiber’s positive charge and superior ability to attract and retain microorganisms are the key reasons it is favored over cotton for environmental cleaning and infection prevention.
Which of the following organisms is associated with a waterborne disease?
Bacillus anthracis
Cytomegalovirus
Nontuberculous mycobacteria
Stachybotrys
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies nontuberculous mycobacteria (NTM) as organisms commonly associated with waterborne exposure. NTM are environmental mycobacteria widely found in natural and treated water sources, including potable water systems, ice machines, showerheads, faucets, and medical equipment rinsed with tap water. Because these organisms are resistant to standard water disinfection methods and can form biofilms, they are particularly well adapted to survive in plumbing systems.
NTM have been implicated in healthcare-associated infections, especially among immunocompromised patients, and may cause pulmonary disease, skin and soft tissue infections, and invasive disease following exposure to contaminated water or medical devices. The Study Guide emphasizes the importance of water management programs and routine surveillance to prevent waterborne transmission of opportunistic pathogens such as NTM and Legionella.
The other answer options are incorrect. Bacillus anthracis is primarily associated with zoonotic and bioterrorism-related exposure, not waterborne transmission. Cytomegalovirus is transmitted through direct contact with bodily fluids rather than water. Stachybotrys is a mold associated with damp indoor environments but is not considered a waterborne pathogen in the context of infection transmission.
Understanding organisms linked to water systems is critical for infection preventionists, as waterborne pathogens present ongoing risks in healthcare facilities and are a key topic on the CIC® exam.
==========
An infection preventionist is preparing an in-service for a new program on total joint replacement. When discussing etiologic agents, which of the following organisms is MOST likely to cause a surgical site infection (SSI) within 60 days of a total hip replacement?
Escherichia coli
Group A streptococci
Pseudomonas aeruginosa
Coagulase-negative staphylococci
The Certification Study Guide (6th edition) identifies coagulase-negative staphylococci (CoNS) as among the most common causes of surgical site infections following orthopedic implant procedures, including total hip replacement. These organisms are part of normal human skin flora and are therefore a frequent source of contamination during surgery, even when aseptic technique is followed. Their importance is heightened in procedures involving prosthetic material because CoNS have a strong ability to adhere to foreign bodies and form biofilms, which protect bacteria from host defenses and antimicrobial therapy.
The study guide emphasizes that SSIs following joint replacement procedures often present within 30 to 60 days postoperatively and are typically caused by gram-positive cocci, particularly Staphylococcus aureus and coagulase-negative staphylococci. CoNS are especially associated with indolent or delayed infections involving implanted devices, making them a critical teaching point in joint replacement programs.
The other organisms listed are less likely causes in this setting. Escherichia coli and Pseudomonas aeruginosa are more commonly associated with gastrointestinal, urinary, or moist environmental sources rather than clean orthopedic procedures. Group A streptococci may cause acute SSIs but are far less common in prosthetic joint infections.
Understanding organism-specific risks allows infection preventionists to target prevention strategies, antimicrobial prophylaxis, and surveillance effectively—key competencies tested on the CIC exam.
Based on the compiled results of learner needs assessments, the staff has an interest in hepatitis B, wound care, and continuing education credits. What should be the infection preventionist’s next step?
Conduct personal interviews with the staff
Offer a lecture on hepatitis B and wound care
Write program goals and objectives
Directly observe behavioral changes
The infection preventionist’s (IP) next step, based on the compiled results of learner needs assessments indicating staff interest in hepatitis B, wound care, and continuing education credits, should be to write program goals and objectives. This step is critical in the educational planning process, as outlined by the Certification Board of Infection Control and Epidemiology (CBIC) guidelines. According to CBIC, effective infection prevention education programs begin with a structured approach that includes defining clear goals and objectives tailored to the identified needs of the learners (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.1 - Develop and implement educational programs). Writing program goals and objectives ensures that the educational content aligns with the staff’s interests and professional development needs, such as understanding hepatitis B prevention, wound care techniques, and earning continuing education credits. This step provides a foundation for designing relevant and measurable outcomes, which can later guide the development of lectures, training materials, or other interventions.
Option A (conduct personal interviews with the staff) is less appropriate as the next step because the needs assessment has already been completed, providing sufficient data on staff interests. Additional interviews might be useful for refining details but are not the immediate priority. Option B (offer a lecture on hepatitis B and wound care) is a subsequent action that follows the establishment of goals and objectives, as delivering content without a structured plan may lack focus or fail to meet educational standards. Option D (directly observe behavioral changes) is an evaluation step that occurs after the education program has been implemented and is not the initial action required.
By starting with program goals and objectives, the IP ensures a systematic approach that adheres to CBIC’s emphasis on evidence-based education and continuous improvement in infection prevention practices. This process also facilitates collaboration with stakeholders to meet accreditation or certification requirements, such as those for continuing education credits.
An infection preventionist is reviewing a wound culture result on a surgery patient. The abdominal wound culture of purulent drainage grew Staphylococcus aureus with the following sensitivity pattern: resistant to penicillin, oxacillin, cephalothin, and erythromycin; susceptible to clindamycin, and vancomycin. The patient is currently being treated with cefazolin. Which of the following is true?
The wound is not infected.
The current therapy is not effective.
Droplet Precautions should be initiated.
This is a methicillin-sensitive S. aureus (MSSA) strain.
The scenario involves a surgical patient with a purulent abdominal wound culture growing Staphylococcus aureus, a common pathogen in surgical site infections (SSIs). The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes accurate interpretation of culture results and antibiotic therapy in the "Identification of Infectious Disease Processes" and "Prevention and Control of Infectious Diseases" domains, aligning with the Centers for Disease Control and Prevention (CDC) guidelines for managing SSIs. The question requires assessing the sensitivity pattern and current treatment to determine the correct statement.
Option B, "The current therapy is not effective," is true. The wound culture shows Staphylococcus aureus resistant to oxacillin, indicating methicillin-resistant S. aureus (MRSA). The sensitivity pattern lists resistance to penicillin, oxacillin, cephalothin, and erythromycin, with susceptibility to clindamycin and vancomycin. Cefazolin, a first-generation cephalosporin, is ineffective against MRSA because resistance to oxacillin (a penicillinase-resistant penicillin) implies cross-resistance to cephalosporins like cefazolin due to altered penicillin-binding proteins (PBPs). The CDC’s "Guidelines for the Prevention of Surgical Site Infections" (2017) and the Clinical and Laboratory Standards Institute (CLSI) standards confirm that MRSA strains are not susceptible to cefazolin, meaning the current therapy is inappropriate and unlikely to resolve the infection, supporting Option B.
Option A, "The wound is not infected," is incorrect. The presence of purulent drainage, a clinical sign of infection, combined with a positive culture for S. aureus, confirms an active wound infection. The CBIC and CDC define purulent discharge as a key indicator of SSI, ruling out this statement. Option C, "Droplet Precautions should be initiated," is not applicable. Droplet Precautions are recommended for pathogens transmitted via respiratory droplets (e.g., influenza, pertussis), not for S. aureus, which is primarily spread by contact. The CDC’s "Guideline for Isolation Precautions" (2007) specifies Contact Precautions for MRSA, not Droplet Precautions, making this false. Option D, "This is a methicillin-sensitive S. aureus (MSSA) strain," is incorrect. Methicillin sensitivity is determined by susceptibility to oxacillin, and the resistance to oxacillin in the culture result classifies this as MRSA, not MSSA. The CDC and CLSI use oxacillin resistance as the defining criterion for MRSA.
The CBIC Practice Analysis (2022) and CDC guidelines stress the importance of aligning antimicrobial therapy with sensitivity patterns to optimize treatment outcomes. The mismatch between cefazolin and the MRSA sensitivity profile confirms that Option B is the correct statement, indicating ineffective current therapy.
A new hospital disinfectant with a 3-minute contact time has been purchased by Environmental Services. The disinfectant will be rolled out across the patient care 3-minute contact time has been purchased by Environmental Services. The disinfectant will be rolled out across the patient care areas. They are concerned about the high cost of the disinfectant. What advice can the infection preventionist provide?
Use the new disinfectant for patient washrooms only.
Use detergents on the floors in patient rooms.
Use detergents on smooth horizontal surfaces.
Use new disinfectant for all surfaces in the patient room.
The scenario involves the introduction of a new hospital disinfectant with a 3-minute contact time, intended for use across patient care areas, but with concerns raised by Environmental Services about its high cost. The infection preventionist’s advice must balance infection control efficacy with cost management, adhering to principles outlined by the Certification Board of Infection Control and Epidemiology (CBIC) and evidence-based practices. The goal is to optimize the disinfectant’s use while ensuring a safe environment. Let’s evaluate each option:
A. Use the new disinfectant for patient washrooms only: Limiting the disinfectant to patient washrooms focuses its use on high-touch, high-risk areas where pathogens (e.g., Clostridioides difficile, norovirus) may be prevalent. However, this approach restricts the disinfectant’s application to a specific area, potentially leaving other patient care surfaces (e.g., bed rails, tables) vulnerable to contamination. While cost-saving, it does not address the broad infection control needs across all patient care areas, making it an incomplete strategy.
B. Use detergents on the floors in patient rooms: Detergents are cleaning agents that remove dirt and organic material but lack the antimicrobial properties of disinfectants. Floors in patient rooms can harbor pathogens, but they are generally considered lower-risk surfaces compared to high-touch areas (e.g., bed rails, doorknobs). Using detergents instead of the new disinfectant on floors could reduce costs but compromises infection control, as floors may still contribute to environmental transmission (e.g., via shoes or equipment). This option is not optimal given the availability of an effective disinfectant.
C. Use detergents on smooth horizontal surfaces: Smooth horizontal surfaces (e.g., tables, counters, overbed tables) are common sites for pathogen accumulation and transmission in patient rooms. Using detergents to clean these surfaces removes organic material, which is a critical first step before disinfection. If the 3-minute contact time disinfectant is reserved for high-touch or high-risk surfaces (e.g., bed rails, call buttons) where disinfection is most critical, this approach maximizes the disinfectant’s efficacy while reducing its overall use and cost. This strategy aligns with CBIC guidelines, which emphasize a two-step process (cleaning followed by disinfection) and targeted use of resources, making it a practical and cost-effective recommendation.
D. Use new disinfectant for all surfaces in the patient room: Using the disinfectant on all surfaces ensures comprehensive pathogen reduction but increases consumption and cost, which is a concern for Environmental Services. While the 3-minute contact time suggests efficiency, overusing the disinfectant on low-risk surfaces (e.g., floors, walls) may not provide proportional infection control benefits and could strain the budget. This approach does not address the cost concern and is less strategic than targeting high-risk areas.
The best advice is C, using detergents on smooth horizontal surfaces to handle routine cleaning, while reserving the new disinfectant for high-touch or high-risk areas where its antimicrobial action is most needed. This optimizes infection prevention, aligns with CBIC’s emphasis on evidence-based environmental cleaning, and addresses the cost concern by reducing unnecessary disinfectant use. The infection preventionist should also recommend a risk assessment to identify priority surfaces for disinfectant application.
CBIC Infection Prevention and Control (IPC) Core Competency Model (updated 2023), Domain IV: Environment of Care, which advocates for targeted cleaning and disinfection based on risk.
CBIC Examination Content Outline, Domain III: Prevention and Control of Infectious Diseases, which includes cost-effective use of disinfectants.
CDC Guidelines for Environmental Infection Control in Healthcare Facilities (2022), which recommend cleaning with detergents followed by targeted disinfection.
Which of the following stains is used to identify mycobacteria?
Acid-fast
Gram
Methylene blue
India ink
Mycobacteria, including species such as Mycobacterium tuberculosis and Mycobacterium leprae, are a group of bacteria known for their unique cell wall composition, which contains a high amount of lipid-rich mycolic acids. This characteristic makes them resistant to conventional staining methods and necessitates the use of specialized techniques for identification. The acid-fast stain is the standard method for identifying mycobacteria in clinical and laboratory settings. This staining technique, developed by Ziehl-Neelsen, involves the use of carbol fuchsin, which penetrates the lipid-rich cell wall of mycobacteria. After staining, the sample is treated with acid-alcohol, which decolorizes non-acid-fast organisms, while mycobacteria retain the red color due to their resistance to decolorization—hence the term "acid-fast." This property allows infection preventionists and microbiologists to distinguish mycobacteria from other bacteria under a microscope.
Option B, the Gram stain, is a common differential staining technique used to classify most bacteria into Gram-positive or Gram-negative based on the structure of their cell walls. However, mycobacteria do not stain reliably with the Gram method due to their thick, waxy cell walls, rendering it ineffective for their identification. Option C, methylene blue, is a simple stain used to observe bacterial morphology or as a counterstain in other techniques (e.g., Gram staining), but it lacks the specificity to identify mycobacteria. Option D, India ink, is used primarily to detect encapsulated organisms such as Cryptococcus neoformans by creating a negative staining effect around the capsule, and it is not suitable for mycobacteria.
The CBIC’s "Identification of Infectious Disease Processes" domain underscores the importance of accurate diagnostic methods in infection control, including the use of appropriate staining techniques to identify pathogens like mycobacteria. The acid-fast stain is specifically recommended by the CDC and WHO for the initial detection of mycobacterial infections, such as tuberculosis, in clinical specimens (CDC, Laboratory Identification of Mycobacteria, 2008). This aligns with the CBIC Practice Analysis (2022), which emphasizes the role of laboratory diagnostics in supporting infection prevention strategies.
Which of the following is the primary advantage of conducting prospective surveillance?
It is an efficient use of surveillance time.
It provides access to complete laboratory data.
It utilizes resources in a cost-effective manner.
It identifies clusters of infection in a timely manner.
The CBIC Certified Infection Control Exam Study Guide (6th edition) describes prospective surveillance as an active, real-time approach to infection surveillance in which patients are monitored as care is being delivered. The primary advantage of this method is its ability to identify infections, trends, and clusters promptly, allowing for early intervention and rapid implementation of control measures.
Because prospective surveillance occurs concurrently with patient care, infection preventionists can detect emerging patterns—such as an increase in device-associated infections or unusual organisms—before they become widespread outbreaks. This timely recognition supports immediate corrective actions, such as reinforcing isolation precautions, modifying clinical practices, or initiating focused investigations, thereby reducing transmission and patient harm.
The other options describe characteristics that are more consistent with retrospective surveillance. Option A and C are incorrect because prospective surveillance is typically more resource- and labor-intensive, not necessarily efficient or cost-effective. Option B is also incorrect because complete laboratory data may not yet be available in real time, whereas retrospective surveillance benefits from finalized records.
For the CIC® exam, it is important to understand that although prospective surveillance requires more resources, its key strength lies in early detection and timely response. The ability to quickly identify clusters of infection and intervene promptly is the defining advantage of prospective surveillance and the reason it is preferred for high-risk settings and priority infections.
A 15-year-old is diagnosed with invasive meningococcal disease. Which of the following should receive chemoprophylaxis?
Household members
A healthcare personnel who was exposed to urine and feces
A school classmate who has shared school supplies
Basketball teammates
The CBIC Certified Infection Control Exam Study Guide (6th edition) clearly outlines recommendations for postexposure chemoprophylaxis following invasive meningococcal disease, which is caused by Neisseria meningitidis. This organism is transmitted through direct contact with respiratory secretions or saliva, such as through kissing, sharing eating utensils, or prolonged close household contact.
Household members are considered high-risk close contacts because they have sustained, close exposure to the patient’s respiratory droplets and oral secretions. As a result, they should receive chemoprophylaxis as soon as possible, ideally within 24 hours of identification of the index case, to prevent secondary cases. This recommendation applies regardless of vaccination status.
The other options do not meet criteria for prophylaxis. Healthcare personnel exposed only to urine or feces (Option B) are not at risk, as N. meningitidis is not transmitted via these routes. Casual school contact or sharing supplies (Option C) does not constitute close exposure to respiratory secretions. Athletic teammates (Option D) generally do not require prophylaxis unless there was direct exposure to saliva (e.g., sharing water bottles or mouthguards).
For CIC® exam preparation, it is essential to recognize that chemoprophylaxis is limited to close contacts with direct exposure to respiratory secretions, with household members being the most consistent and clearly defined group requiring prophylaxis.
A nutrition support team wants to determine whether patients who receive total parenteral nutrition (TPN) at home are at increased risk of central line–associated bloodstream infection (CLABSI) compared with patients who receive TPN in the hospital. The BEST way to compare these two groups is to calculate the:
Percentage of patients in each group who became infected.
Infections per 1,000 central line days in each group.
Number of infections in each group this year compared to last year.
Ratio of infected to noninfected central lines in each group.
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that accurate comparison of healthcare-associated infection risk between groups requires use of standardized, exposure-based rates. For central line–associated bloodstream infections (CLABSIs), the recommended metric is infections per 1,000 central line days, which accounts for the amount of time patients are actually exposed to the risk factor—in this case, the presence of a central venous catheter.
Patients receiving TPN at home and those receiving TPN in the hospital may differ substantially in duration of catheter use, care practices, and patient acuity. Simply comparing percentages or raw numbers of infections fails to adjust for differences in central line utilization and can result in misleading conclusions. By using central line days as the denominator, infection rates are normalized and allow for valid comparisons between populations and settings.
Option A does not account for differences in exposure time. Option C compares different time periods rather than comparing risk between groups. Option D provides a ratio but lacks standardization and is not consistent with accepted surveillance methodology.
The Study Guide reinforces that device-associated infection surveillance—such as CLABSI monitoring—must use device days to assess true risk and guide prevention strategies. Understanding and applying correct epidemiologic measures is a core competency for infection preventionists and a frequently tested concept on the CIC® exam.
==========
An infection preventionist is calculating measures of central tendency regarding duration of a surgical procedure using this data set: 2, 2, 3, 4, and 9. Which of the following statements is correct?
The median is 2.
The mode is 3.
The mean is 4.
The standard deviation is 7.
Measures of central tendency (mean, median, mode) and dispersion (standard deviation) are statistical tools used to summarize data, such as the duration of surgical procedures, which can help infection preventionists identify trends or risks for surgical site infections. The Certification Board of Infection Control and Epidemiology (CBIC) supports the use of data analysis in the "Surveillance and Epidemiologic Investigation" domain, aligning with epidemiological principles outlined by the Centers for Disease Control and Prevention (CDC). The question provides a data set of 2, 2, 3, 4, and 9, and requires determining the correct statement by calculating these measures.
Mean: The mean is the average of the data set, calculated by summing all values and dividing by the number of observations. For the data set 2, 2, 3, 4, and 9:(2 + 2 + 3 + 4 + 9) ÷ 5 = 20 ÷ 5 = 4. Thus, the mean is 4, making Option C correct.
Median: The median is the middle value when the data set is ordered. With five values (2, 2, 3, 4, 9), the middle value is the third number, which is 3. Option A states the median is 2, which is incorrect.
Mode: The mode is the most frequently occurring value. In this data set, 2 appears twice, while 3, 4, and 9 appear once each, making 2 the mode. Option B states the mode is 3, which is incorrect.
Standard Deviation: The standard deviation measures the spread of data around the mean. For a small data set like this, the calculation involves finding the variance (average of squared differences from the mean) and taking the square root. The mean is 4, so the deviations are: (2-4)² = 4, (2-4)² = 4, (3-4)² = 1, (4-4)² = 0, (9-4)² = 25. The sum of squared deviations is 4 + 4 + 1 + 0 + 25 = 34. The variance is 34 ÷ 5 = 6.8, and the standard deviation is ?6.8 ? 2.61 (not 7). Option D states the standard deviation is 7, which is incorrect without further context (e.g., a population standard deviation with n-1 denominator would be ?34 ? 5.83, still not 7).
The CBIC Practice Analysis (2022) and CDC guidelines encourage accurate statistical analysis to inform infection control decisions, such as assessing surgical duration as a risk factor for infections. Based on the calculations, the mean of 4 is the only correct statement among the options, confirming Option C as the answer. Note that the standard deviation of 7 might reflect a miscalculation or misinterpretation (e.g., using a different formula or data set), but with the given data, it does not hold.
Which of the following processes is a critical step in sterile reprocessing of surgical instrumentation?
Send sterile processing disposable and reusable instrumentation for sorting.
Wrap instruments in disposable pads for protection until transporting to sterile processing.
Hold dirty instruments until the evening shift to minimize handling before returning to sterile processing.
Remove bioburden at the point of care and keep instrumentation damp until it reaches the sterile processing department.
A critical principle emphasized in the Certification Study Guide (6th edition) is that instrument reprocessing begins at the point of use, not in the sterile processing department. Immediate removal of gross soil and organic material—referred to as bioburden—prevents drying of blood, tissue, and other debris on instruments. Dried organic material significantly interferes with subsequent cleaning, disinfection, and sterilization processes, reducing the effectiveness of these steps and increasing the risk of surgical site infections.
The study guide explains that instruments should be kept moist or damp after use, typically by using an approved enzymatic spray, damp towel, or transport container, to prevent soil from adhering firmly to surfaces and lumens. This practice protects both the integrity of the instruments and the safety of personnel handling them. Delaying cleaning or allowing instruments to dry increases microbial load and biofilm formation, which are difficult to remove during later processing stages.
The incorrect options conflict with infection prevention standards: holding dirty instruments increases contamination risk; wrapping instruments in pads does not address bioburden; and sending instruments for sorting without point-of-care decontamination violates best practices. Proper point-of-care treatment is foundational to safe, effective sterile processing and is consistently tested on the CIC exam.
A patient with fever, rash, and meningoencephalitis is admitted to the hospital, placed in Droplet Precautions, and started on antibiotic therapy. Bacterial cultures of the blood and spinal fluid are negative, and infection with West Nile virus is strongly suspected by the infectious disease consultant. Appropriate control measures should include:
Administering immunoglobulin to family members.
Discontinuing Droplet Precautions.
Quarantining the family’s pet parakeet.
Continuing present measures.
West Nile virus (WNV) is a mosquito-borne infection. In routine healthcare and household settings, WNV is not spread through coughing, sneezing, or touching and is not transmitted by casual person-to-person contact. Because Transmission-Based Precautions (e.g., Droplet) are used when there is evidence or strong concern for transmission via droplet/contact/airborne routes, WNV suspicion does not justify continuing Droplet Precautions once other droplet-spread causes are no longer suspected.
CDC isolation guidance principles indicate that when there is no evidence for person-to-person transmission by droplet, contact, or airborne routes, Standard Precautions are appropriate. Therefore, the correct action is to discontinue Droplet Precautions and manage the patient using Standard Precautions (hand hygiene and appropriate PPE based on anticipated exposure to blood/body fluids).
The other options are not indicated: immunoglobulin for family members is not a standard infection control measure for WNV, quarantining a pet parakeet is irrelevant to WNV transmission, and “continuing present measures” would unnecessarily maintain Droplet Precautions without a transmission-based indication.
In the current year, cases of tuberculosis (TB) among foreign-born persons accounted for the majority of new TB cases in the United States. The number of states with greater than 50% of cases among foreign-born persons increased from four cases ten years ago to 22 cases in the current year. This information can BEST be used to
heighten awareness among Emergency Department staff.
inform staff who are foreign-born.
educate patients and visitors.
review the TB exposure control plan.
1 and 2 only.
1 and 4 only.
2 and 3 only.
3 and 4 only.
The correct answer is B, "1 and 4 only," indicating that the information can best be used to heighten awareness among Emergency Department (ED) staff and review the TB exposure control plan. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, tuberculosis (TB) remains a significant public health concern, particularly with the increasing proportion of cases among foreign-born persons in the United States. The data showing a rise from four to 22 states with over 50% of TB cases among foreign-born individuals highlights an evolving epidemiological trend that warrants targeted infection prevention strategies (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.1 - Conduct surveillance for healthcare-associated infections and epidemiologically significant organisms).
Heightening awareness among ED staff (option 1) is critical because the ED is often the first point of contact for patients with undiagnosed or active TB, especially those from high-prevalence regions. Increased awareness can improve early identification, isolation, and reporting of potential cases. Reviewing the TB exposure control plan (option 4) is equally important, as it allows the infection preventionist to assess and update protocols—such as ventilation, personal protective equipment (PPE) use, and screening processes—to address the heightened risk posed by the growing number of cases among foreign-born individuals (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.2 - Implement measures to prevent transmission of infectious agents).
Option 2 (inform staff who are foreign-born) is not the best use of this data, as the information pertains to patient demographics rather than staff risk, and targeting staff based on their origin could be inappropriate without specific exposure evidence. Option 3 (educate patients and visitors) is a general education strategy but less directly actionable with this specific epidemiological data, which is more relevant to healthcare worker preparedness and facility protocols. Combining options 1 and 4 aligns with CBIC’s emphasis on using surveillance data to guide prevention and control measures, ensuring a proactive response to the increased TB burden (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.5 - Use data to guide infection prevention and control strategies).
The intensive care unit has noted an increase in patients with ventilator-associated events (VAEs). Which of the following may be contributing to the increase in these events?
Supine position during transport
Daily sedation vacation
Daily weaning assessment
Daily oral care with chlorhexidine
Ventilator-associated events (VAEs) are complications that occur in patients receiving mechanical ventilation and include conditions such as ventilator-associated pneumonia (VAP), pulmonary edema, and atelectasis. The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that patient positioning plays a critical role in preventing aspiration and subsequent respiratory complications in mechanically ventilated patients.
Maintaining patients in a supine position, particularly during transport, increases the risk of aspiration of gastric contents and oropharyngeal secretions. Aspiration is a well-recognized contributing factor to the development of VAEs because it can lead to infection, inflammation, and worsening oxygenation. The Study Guide recommends maintaining the head of the bed elevated (generally 30–45 degrees) whenever feasible, including during care activities and transport, to reduce aspiration risk.
The other options listed—daily sedation vacation, daily weaning assessment, and daily oral care with chlorhexidine—are evidence-based prevention strategies that are part of ventilator care bundles. These interventions are designed to reduce the duration of mechanical ventilation, improve pulmonary function, and decrease microbial colonization, all of which lower the risk of VAEs rather than contribute to them.
Therefore, supine positioning during transport is the most likely factor contributing to an increase in ventilator-associated events and represents a deviation from recommended infection prevention practices.
Which of the following is an example of an outcome measure?
Hand hygiene compliance rate
Adherence to Environmental Cleaning
Rate of multi-drug resistant organisms acquisition
Timing of preoperative antibiotic administration
The correct answer is C, "Rate of multi-drug resistant organisms acquisition," as it represents an example of an outcome measure. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, outcome measures are indicators that reflect the impact or result of infection prevention and control interventions on patient health outcomes or the incidence of healthcare-associated infections (HAIs). The rate of multi-drug resistant organisms (MDRO) acquisition directly measures the incidence of new infections caused by resistant pathogens, which is a key outcome affected by the effectiveness of infection control practices (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.4 - Evaluate the effectiveness of infection prevention and control interventions).
Option A (hand hygiene compliance rate) is an example of a process measure, which tracks adherence to specific protocols or practices intended to prevent infections, rather than the resulting health outcome. Option B (adherence to environmental cleaning) is also a process measure, focusing on the implementation of cleaning protocols rather than the end result, such as reduced infection rates. Option D (timing of preoperative antibiotic administration) is another process measure, assessing the timeliness of an intervention to prevent surgical site infections, but it does not directly indicate the outcome (e.g., infection rate) of that intervention.
Outcome measures, such as the rate of MDRO acquisition, are critical for evaluating the success of infection prevention programs and are often used to guide quality improvement initiatives. This aligns with CBIC’s emphasis on using surveillance data to assess the effectiveness of interventions and inform decision-making (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.5 - Use data to guide infection prevention and control strategies). The focus on MDRO acquisition specifically highlights a significant healthcare challenge, making it a prioritized outcome measure in infection control.
During the last week in June, an emergency department log reveals numerous cases of profuse watery diarrhea in individuals 74 years of age and older. During the same time period, four immunocompromised patients were admitted with possible Cryptosporidium. Which of the following actions should the infection preventionist take FIKST?
Characterize the outbreak by person, place, and time
Increase surveillance facility wide for additional cases
Contact the laboratory to confirm stool identification results
Form a tentative hypothesis about the potential reservoir for this outbreak
When an outbreak of infectious disease is suspected, the first step is to conduct an epidemiologic investigation. This begins with characterizing the outbreak by person, place, and time to establish patterns and trends. This approach, known as descriptive epidemiology, provides critical insights into potential sources and transmission patterns.
Step-by-Step Justification:
Identify Cases and Patterns:
The infection preventionist should analyze patient demographics (person), locations of cases (place), and onset of symptoms (time). This helps in defining the outbreak scope and potential exposure sources?.
Create an Epidemic Curve:
An epidemic curve helps determine whether the outbreak is a point-source or propagated event. This can indicate whether the infection is spreading person-to-person or originating from a common source?.
Compare with Baseline Data:
Reviewing historical data ensures that the observed cases exceed the expected norm, confirming an outbreak?.
Guide Further Investigation:
Establishing basic epidemiologic patterns guides subsequent actions, such as laboratory testing, environmental sampling, and surveillance?.
Why Other Options Are Incorrect:
B. Increase surveillance facility-wide for additional cases:
While enhanced surveillance is important, it should follow the initial characterization of the outbreak. Surveillance without a defined case profile may lead to misclassification and misinterpretation?.
C. Contact the laboratory to confirm stool identification results:
Confirming lab results is essential but comes after defining the outbreak's characteristics. Without an epidemiologic link, testing may yield results that are difficult to interpret?.
D. Form a tentative hypothesis about the potential reservoir for this outbreak:
Hypothesis generation occurs after sufficient epidemiologic data have been collected. Jumping to conclusions without characterization may result in incorrect assumptions and ineffective control measures?.
CBIC Infection Control References:
APIC Text, "Outbreak Investigations," Epidemiology, Surveillance, Performance, and Patient Safety Measures?.
APIC/JCR Infection Prevention and Control Workbook, Chapter 4, Surveillance Program?.
APIC Text, "Investigating Infectious Disease Outbreaks," Guidelines for Epidemic Curve Analysis?.
An infection preventionist is evaluating a new catheter that may decrease the rate of catheter-associated urinary tract infections. Which of the following provides the BEST information to support the selection of this catheter?
Staff member preference and product availability
Product materials and vendor information
Value analysis and information provided by the manufacturer
Cost benefit analysis and safety considerations
The correct answer is D, "Cost benefit analysis and safety considerations," as this provides the best information to support the selection of a new catheter aimed at decreasing the rate of catheter-associated urinary tract infections (CAUTIs). According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, selecting medical devices like catheters for infection prevention involves a comprehensive evaluation that balances efficacy, safety, and economic impact. A cost-benefit analysis assesses the financial implications (e.g., reduced infection rates leading to lower treatment costs) against the cost of the new catheter, while safety considerations ensure the device minimizes patient risk, such as reducing biofilm formation or irritation that contributes to CAUTIs (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.3 - Ensure safe reprocessing of medical equipment). This dual focus provides evidence-based data to justify the catheter’s adoption, aligning with the goal of improving patient outcomes and reducing healthcare-associated infections (HAIs).
Option A (staff member preference and product availability) is subjective and logistical rather than evidence-based, making it insufficient for a decision that impacts infection rates. Option B (product materials and vendor information) offers technical details but lacks the broader context of efficacy and cost-effectiveness needed for a comprehensive evaluation. Option C (value analysis and information provided by the manufacturer) includes a structured assessment of value, but it may be biased toward the manufacturer’s claims and lacks the independent safety and cost-benefit perspective critical for infection prevention decisions.
The emphasis on cost-benefit analysis and safety considerations reflects CBIC’s priority on using data-driven and patient-centered approaches to select interventions that enhance infection control (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.5 - Use data to guide infection prevention and control strategies). This approach ensures the catheter’s selection is supported by robust evidence, optimizing both clinical and economic outcomes in the prevention of CAUTIs.
When conducting a literature search which of the following study designs may provide the best evidence of a direct causal relationship between the experimental factor and the outcome?
A case report
A descriptive study
A case control study
A randomized-controlled trial
To determine the best study design for providing evidence of a direct causal relationship between an experimental factor and an outcome, it is essential to understand the strengths and limitations of each study design listed. The goal is to identify a design that minimizes bias, controls for confounding variables, and establishes a clear cause-and-effect relationship.
A. A case report: A case report is a detailed description of a single patient or a small group of patients with a particular condition or outcome, often including the experimental factor of interest. While case reports can generate hypotheses and highlight rare occurrences, they lack a control group and are highly susceptible to bias. They do not provide evidence of causality because they are observational and anecdotal in nature. This makes them the weakest design for establishing a direct causal relationship.
B. A descriptive study: Descriptive studies, such as cross-sectional or cohort studies, describe the characteristics or outcomes of a population without manipulating variables. These studies can identify associations between an experimental factor and an outcome, but they do not establish causality due to the absence of randomization or control over confounding variables. For example, a descriptive study might show that a certain infection rate is higher in a group exposed to a specific factor, but it cannot prove the factor caused the infection without further evidence.
C. A case control study: A case control study compares individuals with a specific outcome (cases) to those without (controls) to identify factors that may contribute to the outcome. This retrospective design is useful for studying rare diseases or outcomes and can suggest associations. However, it is prone to recall bias and confounding, and it cannot definitively prove causation because the exposure is not controlled or randomized. It is stronger than case reports or descriptive studies but still falls short of establishing direct causality.
D. A randomized-controlled trial (RCT): An RCT is considered the gold standard for establishing causality in medical and scientific research. In an RCT, participants are randomly assigned to either an experimental group (exposed to the factor) or a control group (not exposed or given a placebo). Randomization minimizes selection bias and confounding variables, while the controlled environment allows researchers to isolate the effect of the experimental factor on the outcome. The ability to compare outcomes between groups under controlled conditions provides the strongest evidence of a direct causal relationship. This aligns with the principles of evidence-based practice, which the CBIC (Certification Board of Infection Control and Epidemiology) emphasizes for infection prevention and control strategies.
Based on this analysis, the randomized-controlled trial (D) is the study design that provides the best evidence of a direct causal relationship. This conclusion is consistent with the CBIC's focus on high-quality evidence to inform infection control practices, as RCTs are prioritized in the hierarchy of evidence for establishing cause-and-effect relationships.
CBIC Infection Prevention and Control (IPC) Core Competency Model (updated guidelines, 2023), which emphasizes the use of high-quality evidence, including RCTs, for validating infection control interventions.
CBIC Examination Content Outline, Domain I: Identification of Infectious Disease Processes, which underscores the importance of evidence-based study designs in infection control research.
A nurse claims to have acquired hepatitis A virus infection as the result of occupational exposure. The source patient had an admitting diagnosis of viral hepatitis. Further investigation of this incident reveals a 5-day interval between exposure and onset of symptoms in the nurse. The patient has immunoglobulin G antibodies to hepatitis A. From the evidence, the infection preventionist may correctly conclude which of the following?
The nurse should be given hepatitis A virus immunoglobulin.
The evidence at this time fails to support the nurse's claim.
The patient has serologic evidence of recent hepatitis A viral infection.
The 5-day incubation period is consistent with hepatitis A virus transmission.
The infection preventionist’s (IP) best conclusion, based on the provided evidence, is that the evidence at this time fails to support the nurse's claim of acquiring hepatitis A virus (HAV) infection through occupational exposure. This conclusion is grounded in the clinical and epidemiological understanding of HAV, as aligned with the Certification Board of Infection Control and Epidemiology (CBIC) guidelines. Hepatitis A typically has an incubation period ranging from 15 to 50 days, with an average of approximately 28-30 days, following exposure to the virus (CBIC Practice Analysis, 2022, Domain I: Identification of Infectious Disease Processes, Competency 1.3 - Apply principles of epidemiology). The reported 5-day interval between exposure and symptom onset in the nurse is significantly shorter than the expected incubation period, making it inconsistent with HAV transmission. Additionally, the presence of immunoglobulin G (IgG) antibodies in the source patient indicates past exposure or immunity to HAV, rather than an active or recent infection, which would typically be associated with immunoglobulin M (IgM) antibodies during the acute phase.
Option A (the nurse should be given hepatitis A virus immunoglobulin) is not supported because post-exposure prophylaxis with HAV immunoglobulin is recommended only within 14 days of exposure to a confirmed case with active infection, and the evidence here does not confirm a recent exposure or active case. Option C (the patient has serologic evidence of recent hepatitis A viral infection) is incorrect because IgG antibodies signify past infection or immunity, not a recent infection, which would require IgM antibodies. Option D (the 5-day incubation period is consistent with hepatitis A virus transmission) is inaccurate due to the mismatch with the known incubation period of HAV.
The IP’s role includes critically evaluating epidemiological data to determine the likelihood of transmission events. The discrepancy in the incubation period and the serologic status of the patient suggest that the nurse’s claim may not be substantiated by the current evidence, necessitating further investigation rather than immediate intervention or acceptance of the claim. This aligns with CBIC’s emphasis on accurate identification and investigation of infectious disease processes (CBIC Practice Analysis, 2022, Domain I: Identification of Infectious Disease Processes, Competency 1.2 - Investigate suspected outbreaks or exposures).
Infection Prevention and Control identified a cluster of Aspergillus fumigatus infections in the transplant unit. The infection preventionist (IP) meets with the unit director and Environmental Services director to begin investigation. What information does the IP need from the Environmental Services director?
Date of last terminal clean of the infected patient rooms
Hospital grade disinfectant used on the transplant unit
Use of dust mitigating strategies during floor care
Date of the last cleaning of the fish tank in the waiting room
The correct answer is A, "Date of last terminal clean of the infected patient rooms," as this is the most critical information the infection preventionist (IP) needs from the Environmental Services director to begin the investigation of a cluster of Aspergillus fumigatus infections in the transplant unit. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, Aspergillus fumigatus is an environmental fungus that thrives in areas with poor ventilation, construction dust, or inadequate cleaning, posing a significant risk to immunocompromised patients, such as those in transplant units. A terminal clean—thorough disinfection and cleaning of a patient room after discharge or transfer—is a key infection control measure to eliminate fungal spores and other pathogens (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.4 - Implement environmental cleaning and disinfection protocols). Determining the date of the last terminal clean helps the IP assess whether lapses in cleaning schedules or procedures could have contributed to the cluster, guiding further environmental sampling or process improvements.
Option B (hospital grade disinfectant used on the transplant unit) is relevant to the investigation but is secondary; the IP would need to know the cleaning schedule first to contextualize the disinfectant’s effectiveness. Option C (use of dust mitigating strategies during floor care) is important, as Aspergillus spores can be aerosolized during floor maintenance, but this is a specific procedural detail that follows the initial focus on cleaning history. Option D (date of the last cleaning of the fish tank in the waiting room) is unlikely to be a priority unless evidence suggests a direct link to the transplant unit, which is not indicated here; Aspergillus is more commonly associated with air quality and room cleaning rather than fish tanks.
The focus on the date of the last terminal clean aligns with CBIC’s emphasis on investigating environmental factors in healthcare-associated infection (HAI) clusters, enabling the IP to collaborate with Environmental Services to pinpoint potential sources and implement corrective actions (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.2 - Analyze surveillance data). This step is foundational to controlling the outbreak and protecting vulnerable patients.
A 2-yoar-old girl is admitted with a fractured tibia. At birth, she was diagnosed with congenital cytomegalovirus (CMV). Which of the following barrier precautions is appropriate for healthcare personnel caring for her?
Wear masks and gloves
Wear gloves when handling body fluids
No barrier precautions are needed
Use gowns, masks, gloves, and a private room
Standard Precautions are sufficient for congenital cytomegalovirus (CMV), which means that gloves should be used when handling body fluids. CMV is primarily transmitted via direct contact with saliva, urine, or blood.
Why the Other Options Are Incorrect?
A. Wear masks and gloves – Masks are not necessary unless performing high-risk aerosol-generating procedures.
C. No barrier precautions are needed – Gloves are required when handling bodily fluids to prevent transmission.
D. Use gowns, masks, gloves, and a private room – CMV does not require Contact or Airborne Precautions.
CBIC Infection Control Reference
APIC guidelines state that CMV transmission is prevented using Standard Precautions, primarily with glove use for body fluid contact?.
Which of the following statements describes the MOST important consideration of an infection preventionist when assessing the effectiveness of an infection control action plan?
Re-evaluate the action plan every three years.
Update the plan before the risk assessment is completed.
Develop a timeline and assign responsibilities for the stated action.
Monitor and validate the related outcome and process measures.
Assessing the effectiveness of an infection control action plan is a critical responsibility of an infection preventionist (IP) to ensure that interventions reduce healthcare-associated infections (HAIs) and improve patient safety. The Certification Board of Infection Control and Epidemiology (CBIC) highlights this process within the "Surveillance and Epidemiologic Investigation" and "Performance Improvement" domains, emphasizing the need for ongoing evaluation and data-driven decision-making. The Centers for Disease Control and Prevention (CDC) and other guidelines stress that the ultimate goal of an action plan is to achieve measurable outcomes, such as reduced infection rates, which requires systematic monitoring and validation.
Option D, "Monitor and validate the related outcome and process measures," is the most important consideration. Outcome measures (e.g., infection rates, morbidity, or mortality) indicate whether the action plan has successfully reduced the targeted infection risk, while process measures (e.g., compliance with hand hygiene or proper catheter insertion techniques) assess whether the implemented actions are being performed correctly. Monitoring involves continuous data collection and analysis, while validation ensures the data’s accuracy and relevance to the plan’s objectives. The CBIC Practice Analysis (2022) underscores that effective infection control relies on evaluating both outcomes (e.g., decreased central line-associated bloodstream infections) and processes (e.g., adherence to aseptic protocols), making this a dynamic and essential step. The CDC’s "Compendium of Strategies to Prevent HAIs" (2016) further supports this by recommending regular surveillance and feedback as key to assessing intervention success.
Option A, "Re-evaluate the action plan every three years," suggests a periodic review, which is a good practice for long-term planning but is insufficient as the most important consideration. Infection control requires more frequent assessment (e.g., quarterly or annually) to respond to emerging risks or outbreaks, making this less critical than ongoing monitoring. Option B, "Update the plan before the risk assessment is completed," is illogical and counterproductive. Updating a plan without a completed risk assessment lacks evidence-based grounding, undermining the plan’s effectiveness and contradicting the CBIC’s emphasis on data-driven interventions. Option C, "Develop a timeline and assign responsibilities for the stated action," is an important initial step in implementing an action plan, ensuring structure and accountability. However, it is a preparatory activity rather than the most critical factor in assessing effectiveness, which hinges on post-implementation evaluation.
The CBIC Practice Analysis (2022) and CDC guidelines prioritize outcome and process monitoring as the cornerstone of infection control effectiveness, enabling IPs to adjust strategies based on real-time evidence. Thus, Option D represents the most important consideration for assessing an infection control action plan’s success.
The expectation to call out or speak up when an infection prevention lapse is observed is an example of
implementation of human factors.
honest disclosure of a safety event.
a blaming and shaming safety culture.
a safety culture with reciprocal accountability.
A safety culture with reciprocal accountability emphasizes mutual responsibility for maintaining safe practices, encouraging staff at all levels to "speak up" or "stop the line" when they observe risky practices. This concept reflects a learning organization and a just culture that supports open communication and proactive risk mitigation.
According to the APIC Text, a strong safety culture is described as one where:
“The leadership can expect staff members to call out or stop the line when they see risk, and staff can expect leadership to listen and act.”
This dynamic reflects reciprocal accountability.
Other options are less accurate:
A. Human factors refer to system design, not behavioral accountability.
B. Honest disclosure of a safety event is about post-event transparency, not real-time intervention.
C. A blaming and shaming culture is antithetical to safety culture principles.
In evaluating the infection control and ventilation measures for operating rooms the Infection Preventionist should know that the air changes per hour (ACH) should be maintained at greater than or equal to 15 ACH. How many of these changes should be fresh air?
Greater than or equal to 3
Greater than or equal to 5
Greater than or equal to 6
Greater than or equal to 7
In operating rooms, a minimum of 15 air changes per hour (ACH) is required, with at least 3 of those ACH being from fresh or outdoor air. This requirement helps reduce microbial contamination and provides a clean surgical environment.
According to the APIC Text:
"In each, air should flow out of the room and the minimum ACH should be 15, with three of these ACH being fresh or outdoor air."
This aligns with design specifications outlined in the 2006 Guidelines for design and construction of health care facilities.
Based on the scenarios, when should an infection preventionist suspect an outbreak?
Three positive routine environmental cultures of Staphylococcus aureus from the bone marrow transplant unit
Detection of three ventilator-associated pneumonia cases among patients in the intensive care unit (ICU) after updated case definition implementation
Increase in the number of Klebsiella pneumoniae carbapenemase–producing isolates in the ICU after implementation of new minimum inhibitory concentration breakpoints
Detection of three positive blood cultures with methicillin-resistant Staphylococcus aureus in the cardiac ICU for patients who underwent cardiac surgery in the same week
The Certification Study Guide (6th edition) emphasizes that an outbreak should be suspected when there is an unexpected clustering of infections by time, place, and person, particularly when cases share a common exposure or procedure. Option D meets all key criteria for outbreak suspicion: the same organism (methicillin-resistant Staphylococcus aureus), the same location (cardiac ICU), a common procedure (cardiac surgery), and a tight time frame (same week). This constellation strongly suggests possible transmission related to surgical practices, postoperative care, or shared equipment.
The other scenarios reflect situations that do not necessarily indicate an outbreak. Routine environmental cultures are not recommended for outbreak detection and often do not correlate with patient infection risk. An apparent increase in ventilator-associated pneumonia following implementation of a new case definition is likely due to surveillance artifact, not true transmission. Similarly, increases in carbapenemase-producing Klebsiella pneumoniae after adoption of new laboratory breakpoints reflect diagnostic changes, not an epidemiologic event.
The study guide stresses the importance of distinguishing true outbreaks from pseudo-outbreaks caused by changes in definitions, testing methods, or surveillance intensity. CIC exam questions frequently test this concept. Recognizing a true outbreak requires linking cases through epidemiologic characteristics—not simply increases in numbers.
Prompt recognition of true outbreaks enables timely investigation, implementation of control measures, and prevention of further transmission.
An example of active learning is:
Listening to a lecture.
Reading policies.
Exploring case studies.
Watching a recorded presentation.
Active learning is a core educational principle emphasized in the Education and Research domain of the CBIC Certified Infection Control Exam Study Guide (6th edition). Active learning requires the learner to engage cognitively with the material through analysis, problem-solving, and application of knowledge, rather than passively receiving information. Exploring case studies is a classic example of active learning because it requires participants to apply infection prevention principles to real-world or simulated scenarios, interpret data, evaluate risks, and make evidence-based decisions.
The Study Guide highlights that adult learners—such as infection preventionists and healthcare professionals—retain knowledge more effectively when learning activities are interactive and practice-oriented. Case studies encourage critical thinking by presenting complex clinical or operational situations that mirror challenges encountered in infection prevention practice, such as outbreak investigations, surveillance interpretation, or policy implementation. This method supports deeper understanding and long-term retention.
In contrast, listening to lectures, reading policies, or watching recorded presentations are considered passive learning activities. While these methods are valuable for introducing foundational knowledge or disseminating information, they do not actively involve the learner in applying or synthesizing information. The Study Guide specifically notes that combining passive methods with active strategies—such as case discussions, simulations, and problem-based learning—enhances competency development and performance improvement in infection prevention programs.
This distinction is frequently tested on the CIC® exam, making recognition of active learning strategies essential for exam success.
An infection preventionist (IP) receives a phone call from a local health department alerting the hospital of the occurrence of a sewer main break. Contamination of the city water supply is a possibility. Which of the following actions should the IP perform FIRST?
Notify the Emergency and Admissions departments to report diarrhea cases to infection control.
Review microbiology laboratory reports for enteric organisms in the past week.
Contact the Employee Health department and ask for collaboration in case-finding.
Review the emergency preparedness plan with engineering for sources of potable water.
The correct answer is B, "Review microbiology laboratory reports for enteric organisms in the past week," as this is the first action the infection preventionist (IP) should perform following the alert of a sewer main break and potential contamination of the city water supply. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, a rapid assessment of existing data is a critical initial step in investigating a potential waterborne outbreak. Reviewing microbiology laboratory reports for enteric organisms (e.g., Escherichia coli, Salmonella, or Shigella) helps the IP identify any recent spikes in infections that could indicate water supply contamination, providing an evidence-based starting point for the investigation (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.2 - Analyze surveillance data). This step leverages available hospital data to assess the scope and urgency of the situation before initiating broader actions.
Option A (notify the Emergency and Admissions departments to report diarrhea cases to infection control) is an important subsequent step to enhance surveillance, but it relies on proactive reporting and does not provide immediate evidence of an ongoing issue. Option C (contact the Employee Health department and ask for collaboration in case-finding) is valuable for involving additional resources, but it should follow the initial data review to prioritize case-finding efforts based on identified trends. Option D (review the emergency preparedness plan with engineering for sources of potable water) is a critical preparedness action, but it is more relevant once contamination is confirmed or as a preventive measure, not as the first step in assessing the current situation.
The focus on reviewing laboratory reports aligns with CBIC’s emphasis on using surveillance data to guide infection prevention responses, enabling the IP to quickly determine if the sewer main break has already impacted patient health and to escalate actions accordingly (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.1 - Conduct surveillance for healthcare-associated infections and epidemiologically significant organisms). This approach is consistent with CDC guidelines for responding to waterborne outbreak alerts (CDC Environmental Public Health Guidelines, 2020).
Essential knowledge, behaviors, and skills that an individual should possess and demonstrate to practice in a specific discipline defines which of the following?
Certification
Competence
Knowledge
Training
The correct answer is B, "Competence," as it defines the essential knowledge, behaviors, and skills that an individual should possess and demonstrate to practice in a specific discipline. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, competence encompasses the integrated application of knowledge, skills, and behaviors required to perform effectively in a professional role, such as infection prevention and control. Competence goes beyond mere knowledge or training by including the ability to apply these attributes in real-world scenarios, ensuring safe and effective practice (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.3 - Assess competence of healthcare personnel). This holistic definition is critical in healthcare settings, where demonstrated competence—through actions like proper hand hygiene or outbreak management—directly impacts patient safety and infection prevention outcomes.
Option A (certification) refers to a formal recognition or credential (e.g., CIC certification) that validates an individual’s qualifications, but it is an outcome or process rather than the definition of the underlying abilities. Option C (knowledge) represents the theoretical understanding or factual basis of a discipline, which is a component of competence but not the full scope that includes behaviors and skills. Option D (training) involves the education or instruction provided to develop skills and knowledge, serving as a means to achieve competence rather than defining it.
The focus on competence aligns with CBIC’s emphasis on ensuring that healthcare personnel are equipped to meet the demands of infection prevention through a combination of education, practice, and evaluation (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.2 - Evaluate the effectiveness of educational programs). This definition supports the development of professionals who can adapt and perform effectively in dynamic healthcare environments.
An infection preventionist is utilizing the Shewhart/Deming cycle in an infection control program performance improvement project. In which of the following steps are the results of the interventions compared with the original goal?
Do
Act
Plan
Study
The correct answer is D, "Study," as this is the step in the Shewhart/Deming cycle (commonly known as the Plan-Do-Study-Act [PDSA] cycle) where the results of the interventions are compared with the original goal. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, the PDSA cycle is a systematic approach to quality improvement, widely used in infection control programs to test and refine interventions. The cycle consists of four stages: Plan (designing the intervention and setting goals), Do (implementing the intervention on a small scale), Study (analyzing the data and comparing outcomes against the original goal), and Act (standardizing successful changes or adjusting based on findings) (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.2 - Evaluate the effectiveness of educational programs). The Study phase is critical for assessing whether the intervention achieved the intended reduction in infection rates or other performance metrics, providing evidence to guide the next steps.
Option A (Do) involves the execution of the planned intervention, focusing on implementation rather than evaluation, so it does not include comparing results. Option B (Act) is the final step where successful interventions are implemented on a broader scale or adjustments are made, but it follows the comparison made in the Study phase. Option C (Plan) is the initial stage of setting objectives and designing the intervention, which occurs before any results are available for comparison.
The emphasis on the Study phase aligns with CBIC’s focus on using data to evaluate the effectiveness of infection prevention strategies, ensuring that performance improvement projects are evidence-based and goal-oriented (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.4 - Evaluate the effectiveness of infection prevention and control interventions). This step enables the infection preventionist to determine if the original goal—such as reducing healthcare-associated infections—was met, facilitating continuous improvement.
The BEST choice for surgical instrument cleaning and material compatibility is a detergent solution with:
An acidic pH
A neutral pH
Sodium hypochlorite
Quaternary ammonium compounds
The Certification Study Guide (6th edition) emphasizes that the primary goal of surgical instrument cleaning is to remove organic and inorganic soil while preserving the integrity and functionality of the instrument. For this reason, detergents with a neutral pH are considered the best choice for routine surgical instrument cleaning and material compatibility.
Neutral pH detergents are effective at removing blood, tissue, and other organic matter without causing corrosion, pitting, or degradation of metals, plastics, seals, and coatings commonly used in surgical instruments. The study guide notes that repeated exposure to harsh chemical environments can damage instruments, compromise device performance, and shorten instrument lifespan—ultimately affecting patient safety and increasing replacement costs.
Acidic detergents may be used selectively for removal of mineral deposits or water scale but are not appropriate for routine cleaning due to their corrosive potential. Sodium hypochlorite (bleach) is strongly discouraged for surgical instruments because it is highly corrosive and can rapidly damage stainless steel. Quaternary ammonium compounds are low-level disinfectants and are not suitable for cleaning critical or semi-critical medical devices prior to disinfection or sterilization.
This question reflects a high-yield CIC exam principle: effective cleaning must balance soil removal with material compatibility. Neutral pH detergents best meet both requirements and are widely recommended by manufacturers and reprocessing standards for surgical instrumentation.
Endemic infection rate refers to
Disease that overwhelms the usual healthcare system.
The usual presence of a disease in a specific population or geographical area.
An outbreak of disease much greater than expected in a specific population or group.
The occurrence of more cases of a disease than expected in a given area or among a specific group.
The CBIC Certified Infection Control Exam Study Guide (6th edition) defines endemic infection rate as the constant or usual presence of a disease within a specific population, geographic area, or healthcare setting. An endemic level represents the baseline or expected frequency of disease occurrence over time, allowing infection preventionists to distinguish normal disease patterns from unusual increases that may signal outbreaks or epidemics.
Option B accurately reflects this definition by describing the expected and stable presence of a disease within a defined population or location. Endemic infections may persist at low or predictable levels and do not necessarily indicate a failure of infection prevention practices. Examples include seasonal influenza in the community or baseline rates of certain healthcare-associated infections within a facility.
Option A refers to a pandemic or healthcare system overload, not endemic disease. Options C and D describe outbreaks or epidemics, which involve a sudden increase in cases above the expected endemic level. These terms imply deviation from baseline and require investigation and intervention.
Understanding endemic rates is critical for infection prevention and surveillance because they provide the comparison point for identifying trends, clusters, and outbreaks. Surveillance data are interpreted against endemic baselines to determine whether changes reflect random variation or meaningful increases requiring action.
For the CIC® exam, recognizing epidemiologic terminology is essential. Endemic infection rate specifically refers to the usual or expected presence of disease, making option B the correct answer.
When designing a physical construction containment barrier to contain dust as well as potentially infectious microorganisms generated, reduced air pressure in the contained space relative to adjacent occupied spaces results in airflow from the:
Exhaust into the contained work space and then into the clean adjacent space.
Contained work space into the clean adjacent space and then out of the exhaust.
Clean adjacent space into the contained work space and then out the exhaust.
Clean adjacent space into the contained work space and then directly back into the building.
The Certification Study Guide (6th edition) explains that during construction, renovation, or maintenance activities in healthcare facilities, negative (reduced) air pressure within the contained work area is a critical engineering control to prevent the spread of dust and potentially infectious microorganisms. When the pressure inside the containment is lower than in adjacent occupied areas, air naturally flows from areas of higher pressure to areas of lower pressure.
As a result, airflow moves from the clean adjacent space into the contained work space, rather than allowing contaminated air to escape outward. Once inside the containment, the air is then exhausted directly to the outside of the building or through appropriate filtration systems. This airflow pattern protects patients, visitors, and healthcare personnel in occupied areas by preventing construction-related contaminants—such as fungal spores (e.g., Aspergillus)—from spreading into patient care environments.
The study guide emphasizes that this principle is foundational to Infection Control Risk Assessments (ICRAs) and construction containment planning. Improper airflow direction can result in airborne contamination and has been associated with outbreaks, particularly among immunocompromised patients.
The incorrect options either reverse the airflow direction or allow contaminated air to re-enter the building, both of which violate infection prevention standards. Understanding airflow dynamics and pressure differentials is a frequently tested concept on the CIC exam and is essential for ensuring safe construction practices in healthcare facilities.
Working with public health agencies to collect and analyze indicators that might signal an increase in community illness is an example of which type of surveillance?
Passive
Active
Syndromic
Targeted
Surveillance is a critical tool in infection prevention and control, used to monitor disease trends and guide public health responses. The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes the "Surveillance and Epidemiologic Investigation" domain, which aligns with the Centers for Disease Control and Prevention (CDC) "Principles of Epidemiology in Public Health Practice" (3rd Edition, 2012). The question describes a process of collecting and analyzing indicators to signal an increase in community illness, requiring identification of the appropriate surveillance type among the options provided.
Option C, "Syndromic," is the correct answer. Syndromic surveillance involves monitoring non-specific health indicators or symptoms (e.g., fever, respiratory complaints, or gastrointestinal issues) that may precede a formal diagnosis, aiming to detect potential outbreaks or increases in community illness early. The CDC defines syndromic surveillance as the real-time or near-real-time collection, analysis, and interpretation of health-related data to provide actionable information, often in collaboration with public health agencies. This approach uses data from sources like emergency department visits, over-the-counter medication sales, or absenteeism reports to identify trends before laboratory confirmation, making it well-suited to the described scenario of signaling community illness increases.
Option A, "Passive," involves healthcare providers or laboratories reporting cases to public health authorities on a voluntary or mandatory basis without active prompting (e.g., routine notifiable disease reporting). While passive surveillance contributes to baseline data, it is less proactive and not specifically designed to signal early increases in illness, making it less fitting. Option B, "Active," entails public health officials actively seeking data from healthcare facilities or providers (e.g., calling to confirm cases during an outbreak). This is more resource-intensive and typically used for specific investigations rather than ongoing community trend monitoring, which aligns better with syndromic methods. Option D, "Targeted," refers to surveillance focused on a specific population, disease, or event (e.g., monitoring TB in a high-risk group). The scenario’s broad focus on community illness indicators does not suggest a targeted approach.
The CBIC Practice Analysis (2022) and CDC guidelines highlight syndromic surveillance as a key strategy for early detection of community-wide health threats, often involving collaboration with public health agencies. Option C best matches the described activity of analyzing indicators to signal illness increases, making it the correct choice.
Which water type is suitable for drinking yet may still be a risk for disease transmission?
Purified water
Grey water
Potable water
Distilled water
To determine which water type is suitable for drinking yet may still pose a risk for disease transmission, we need to evaluate each option based on its definition, treatment process, and potential for contamination, aligning with infection control principles as outlined by the Certification Board of Infection Control and Epidemiology (CBIC).
A. Purified water: Purified water undergoes a rigorous treatment process (e.g., reverse osmosis, distillation, or deionization) to remove impurities, contaminants, and microorganisms. This results in water that is generally safe for drinking and has a very low risk of disease transmission when properly handled and stored. However, if the purification process is compromised or if contamination occurs post-purification (e.g., due to improper storage or distribution), there could be a theoretical risk. Nonetheless, purified water is not typically considered a primary source of disease transmission under standard conditions.
B. Grey water: Grey water refers to wastewater generated from domestic activities such as washing dishes, laundry, or bathing, which may contain soap, food particles, and small amounts of organic matter. It is not suitable for drinking due to its potential contamination with pathogens (e.g., bacteria, viruses) and chemicals. Grey water is explicitly excluded from potable water standards and poses a significant risk for disease transmission, making it an unsuitable choice for this question.
C. Potable water: Potable water is water that meets regulatory standards for human consumption, as defined by organizations like the World Health Organization (WHO) or the U.S. Environmental Protection Agency (EPA). It is treated to remove harmful pathogens and contaminants, making it safe for drinking under normal circumstances. However, despite treatment, potable water can still pose a risk for disease transmission if the distribution system is contaminated (e.g., through biofilms, cross-connections, or inadequate maintenance of pipes). Outbreaks of waterborne diseases like Legionnaires' disease or gastrointestinal infections have been linked to potable water systems, especially in healthcare settings. This makes potable water the best answer, as it is suitable for drinking yet can still carry a risk under certain conditions.
D. Distilled water: Distilled water is produced by boiling water and condensing the steam, which removes most impurities, minerals, and microorganisms. It is highly pure and safe for drinking, often used in medical and laboratory settings. Similar to purified water, the risk of disease transmission is extremely low unless contamination occurs after distillation due to improper handling or storage. Like purified water, it is not typically associated with disease transmission risks in standard use.
The key to this question lies in identifying a water type that is both suitable for drinking and has a documented potential for disease transmission. Potable water fits this criterion because, while it is intended for consumption and meets safety standards, it can still be a vector for disease if the water supply or distribution system is compromised. This is particularly relevant in infection control, where maintaining water safety in healthcare facilities is a critical concern addressed by CBIC guidelines.
CBIC Infection Prevention and Control (IPC) Core Competency Model (updated 2023), Domain III: Prevention and Control of Infectious Diseases, which highlights the importance of water safety and the risks of contamination in potable water systems.
CBIC Examination Content Outline, Domain IV: Environment of Care, which includes managing waterborne pathogens (e.g., Legionella) in potable water supplies.
A 21-ycnr-old college student was admitted with a high fever. The Emergency Department physician be gan immediate treatment with intravenous vancomycin and ceftriaxone while awaiting blood, urine, and cerebrospinal fluid cultures. The following day. the cultures of both the blood and the cerebrospinal fluid were reported to be growing meningococci. The patient was placed on precautions on admission. Which of the following is correct?
Droplet precautions may be discontinued after 24 hours of therapy.
Droplet precautions must continue
Airborne precautions may be discontinued after 24 hours of therapy.
Airborne precautions must continue.
Meningococcal infections, such as Neisseria meningitidis, are transmitted via respiratory droplets. According to APIC and CDC guidelines, patients with meningococcal disease should be placed on Droplet Precautions upon admission. These precautions can be discontinued after 24 hours of effective antibiotic therapy.
Why the Other Options Are Incorrect?
B. Droplet precautions must continue – Droplet Precautions are not needed beyond 24 hours of appropriate therapy because treatment rapidly reduces infectiousness.
C. Airborne precautions may be discontinued after 24 hours of therapy – Meningococcal infection is not airborne, so Airborne Precautions are never required.
D. Airborne precautions must continue – Incorrect because meningococci do not transmit via airborne particles.
CBIC Infection Control Reference
According to APIC guidelines, Droplet Precautions should be maintained for at least 24 hours after effective antibiotic therapy initiation?.
Steam sterilization should be validated with which of the following organisms?
Geobacillus stearothermophilus
Staphylococcus aureus
Bacillus anthracis
Bacillus atrophaeus
The CBIC Certified Infection Control Exam Study Guide (6th edition) clearly states that steam sterilization (moist heat sterilization) must be validated using biological indicators containing Geobacillus stearothermophilus spores. This organism is selected because its spores are highly resistant to moist heat, making them an ideal challenge organism for assessing the effectiveness of steam sterilization processes.
Biological indicators are used to confirm that sterilization conditions—such as temperature, pressure, and exposure time—are sufficient to achieve microbial inactivation. Geobacillus stearothermophilus thrives at high temperatures and demonstrates strong resistance to steam, so if these spores are destroyed, it provides high confidence that other less-resistant microorganisms, including bacteria, viruses, and fungi, have also been eliminated.
The other options are incorrect for steam sterilization validation. Staphylococcus aureus is a vegetative bacterium and is far less resistant than bacterial spores. Bacillus anthracis is not used as a biological indicator due to safety concerns and lack of standardization. Bacillus atrophaeus is used as the biological indicator for dry heat and ethylene oxide sterilization, not steam.
Understanding which biological indicators correspond to specific sterilization modalities is a high-yield topic on the CIC® exam and is essential for ensuring compliance with evidence-based sterilization and disinfection standards.
=======
Immediate use steam sterilization is NOT recommended for implantable items requiring immediate use because
the high temperature may damage the items.
chemical indicators may not be accurate at high temperatures.
results of biologic indicators are unavailable prior to use of the item.
the length of time is inadequate for the steam to penetrate the pack.
The correct answer is C, "results of biologic indicators are unavailable prior to use of the item," as this is the primary reason immediate use steam sterilization (IUSS) is not recommended for implantable items requiring immediate use. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, IUSS is a process used for sterilizing items needed urgently when no other sterile options are available, typically involving a shortened cycle (e.g., flash sterilization). However, for implantable items—such as orthopedic hardware or prosthetic devices—ensuring absolute sterility is critical due to the risk of deep infection. Biologic indicators (BIs), which contain highly resistant spores to verify sterilization efficacy, require incubation (typically 24-48 hours) to confirm the kill, but IUSS does not allow time for BI results to be available before the item is used (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.3 - Ensure safe reprocessing of medical equipment). This lack of immediate verification poses a significant infection risk, making IUSS inappropriate for implants, as per AAMI ST79 standards.
Option A (the high temperature may damage the items) is a consideration for some heat-sensitive materials, but modern IUSS cycles are designed to minimize damage, and this is not the primary reason for the restriction on implants. Option B (chemical indicators may not be accurate at high temperatures) is incorrect, as chemical indicators (e.g., color-changing strips) are reliable at high temperatures and serve as an immediate check, though they are not a substitute for BIs. Option D (the length of time is inadequate for the steam to penetrate the pack) is not the main issue, as IUSS cycles are optimized for penetration, though the shortened time may be a secondary concern; the unavailability of BI results remains the decisive factor.
The focus on biologic indicator results aligns with CBIC’s emphasis on ensuring the safety and sterility of reprocessed medical devices, particularly for high-risk implantable items (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.5 - Evaluate the environment for infection risks). This recommendation is supported by AAMI and CDC guidelines, which prioritize BI confirmation for implants to prevent healthcare-associated infections (AAMI ST79:2017, CDC Sterilization Guidelines, 2019).
A hospital is experiencing an increase in multidrug-resistant Acinetobacter baumannii infections in the intensive care unit (ICU). The infection preventionist's FIRST action should be to:
Implement universal contact precautions for all ICU patients.
Conduct an epidemiologic investigation to identify potential sources.
Perform environmental sampling to detect Acinetobacter on surfaces.
Initiate decolonization protocols for all ICU patients.
Epidemiologic Investigation:
The first step in an outbreak response is to characterize cases by person, place, and time?.
Identifying common exposures (e.g., ventilators, catheters, or contaminated surfaces) helps determine the source?.
Why Other Options Are Incorrect:
A. Universal contact precautions: Premature; precautions should be tailored based on transmission patterns.
C. Environmental sampling: Should be done after identifying epidemiologic links.
D. Decolonization protocols: Not routinely recommended for Acinetobacter outbreaks.
CBIC Infection Control References:
CIC Study Guide, "Epidemiologic Investigations in Outbreaks," Chapter 4?.
When describing the differences between colonization and infection, the infection preventionist should define colonization as
Tissue invasion by organisms without tissue damage.
Tissue injury by normal flora associated with local reaction.
The presence and growth of organisms without tissue invasion.
The presence and growth of opportunistic organisms with cellular change.
The CBIC Certified Infection Control Exam Study Guide (6th edition) clearly distinguishes colonization from infection, a foundational concept in infection prevention and healthcare epidemiology. Colonization is defined as the presence and multiplication of microorganisms on or within a host without tissue invasion, damage, or clinical signs of disease. Individuals who are colonized do not exhibit symptoms and typically do not mount an inflammatory response.
Option C accurately reflects this definition and is the correct answer. Colonized organisms may be part of normal flora or may be potentially pathogenic organisms such as Staphylococcus aureus or multidrug-resistant organisms. Although colonization does not cause illness, colonized individuals can serve as reservoirs for transmission and may later develop infection if host defenses are compromised.
Option A is incorrect because tissue invasion, even without visible damage, represents infection rather than colonization. Option B describes infection caused by normal flora with an inflammatory response. Option D includes cellular change, which indicates tissue response and therefore infection.
For the CIC® exam, it is essential to understand that colonization involves microbial presence without host response, while infection requires tissue invasion and a corresponding inflammatory or immune reaction. This distinction is critical for surveillance definitions, isolation decisions, antimicrobial stewardship, and patient education.
An infection preventionist is notified of a patient with Gram negative diplococci from a cerebral spinal fluid specimen. The patient was intubated during ambulance transport and intravenous lines are placed after arrival to the Emergency Department (ED). The patient was immediately placed in Droplet Precautions upon admission to the ED. Which of the following statements is true regarding the need for evaluating exposure to communicable illness?
Follow-up evaluation is not required for this laboratory finding.
ED personnel should be evaluated for possible exposure.
Ambulance personnel should be evaluated for possible exposure.
Follow-up evaluation is not necessary as the appropriate precautions were promptly instituted.
The correct answer is C, "Ambulance personnel should be evaluated for possible exposure," as this statement is true regarding the need for evaluating exposure to communicable illness. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, the presence of Gram negative diplococci in a cerebral spinal fluid (CSF) specimen is suggestive of a serious bacterial infection, most likely Neisseria meningitidis, which causes meningococcal disease. This condition is highly contagious and can be transmitted through respiratory droplets or direct contact with respiratory secretions, particularly during procedures like intubation (CBIC Practice Analysis, 2022, Domain I: Identification of Infectious Disease Processes, Competency 1.1 - Identify infectious disease processes). The patient was intubated during ambulance transport, creating a potential aerosol-generating procedure (AGP) that could have exposed ambulance personnel to infectious droplets before Droplet Precautions were instituted upon arrival at the Emergency Department (ED). Therefore, evaluating ambulance personnel for possible exposure is necessary to assess their risk and determine if post-exposure prophylaxis (e.g., antibiotics) or monitoring is required.
Option A (follow-up evaluation is not required for this laboratory finding) is incorrect because the identification of Gram negative diplococci in CSF is a critical finding that warrants investigation due to the potential for meningococcal disease, a reportable and transmissible condition. Option B (ED personnel should be evaluated for possible exposure) is less applicable since the patient was immediately placed in Droplet Precautions upon ED admission, minimizing exposure risk to ED staff after that point, though it could be considered if exposure occurred before precautions were fully implemented. Option D (follow-up evaluation is not necessary as the appropriate precautions were promptly instituted) is inaccurate because the prompt institution of Droplet Precautions in the ED does not retroactively address the exposure risk during ambulance transport, where precautions were not in place.
The focus on evaluating ambulance personnel aligns with CBIC’s emphasis on identifying and mitigating transmission risks associated with communicable diseases, particularly in high-risk settings like ambulance transport (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.2 - Implement measures to prevent transmission of infectious agents). This step is supported by CDC guidelines, which recommend exposure evaluation and prophylaxis for close contacts of meningococcal disease cases (CDC Meningococcal Disease Management, 2021).
The infection preventionist (IP) is working with Environmental Services to evaluate a new disinfectant for purchase by the facility. With which of the following should the IP be MOST concerned?
Safety of the product
Vendor knowledge of product
Vendor proximity to the facility
Staff preference
When evaluating a new disinfectant, the infection preventionist's primary concern must be the safety and effectiveness of the product. This includes ensuring the product is EPA-registered, effective against targeted pathogens, safe for both the environment and users, and compliant with regulatory guidelines.
From the APIC/JCR Workbook, key considerations include:
“Organizations should evaluate each product to ensure that it can be used safely and include a review of dilutions, storage, shelf life, PPE needed, and disposal and ventilation requirements to ensure that OSHA, EPA, or local requirements are met”.
The CBIC Study Guide reinforces that:
"Safety and efficacy are critical factors in evaluating new products, with particular emphasis on infection prevention and user safety".
The other options, while relevant, are not the most critical factors in determining product adoption from an infection control standpoint.
Following recent renovations on an oncology unit, three patients were identified with Aspergillus infections. The infections were thought to be facility-acquired. Appropriate environmental microbiological monitoring would be to culture the:
Air
Ice
Carpet
Aerators
The scenario describes an outbreak of Aspergillus infections among three patients on an oncology unit following recent renovations, with the infections suspected to be facility-acquired. Aspergillus is a mold commonly associated with environmental sources, particularly airborne spores, and its presence in immunocompromised patients (e.g., oncology patients) poses a significant risk. The infection preventionist must identify the appropriate environmental microbiological monitoring strategy, guided by the Certification Board of Infection Control and Epidemiology (CBIC) and CDC recommendations. Let’s evaluate each option:
A. Air: Aspergillus species are ubiquitous molds that thrive in soil, decaying vegetation, and construction dust, and they are primarily transmitted via airborne spores. Renovations can disturb these spores, leading to aerosolization and inhalation by vulnerable patients. Culturing the air using methods such as settle plates, air samplers, or high-efficiency particulate air (HEPA) filtration monitoring is a standard practice to detect Aspergillus during construction or post-renovation in healthcare settings, especially oncology units where patients are at high risk for invasive aspergillosis. This aligns with CBIC’s emphasis on environmental monitoring for airborne pathogens, making it the most appropriate choice.
B. Ice: Ice can be a source of contamination with bacteria (e.g., Pseudomonas, Legionella) or other pathogens if improperly handled or stored, but it is not a typical reservoir for Aspergillus, which is a mold requiring organic material and moisture for growth. While ice safety is important in infection control, culturing ice is irrelevant to an Aspergillus outbreak linked to renovations and is not a priority in this context.
C. Carpet: Carpets can harbor dust, mold, and other microorganisms, especially in high-traffic or poorly maintained areas. Aspergillus spores could theoretically settle in carpet during renovations, but carpets are not a primary source of airborne transmission unless disturbed (e.g., vacuuming). Culturing carpet might be a secondary step if air sampling indicates widespread contamination, but it is less direct and less commonly recommended as the initial monitoring site compared to air sampling.
D. Aerators: Aerators (e.g., faucet aerators) can harbor waterborne pathogens like Pseudomonas or Legionella due to biofilm formation, but Aspergillus is not typically associated with water systems unless there is significant organic contamination or aerosolization from water sources (e.g., cooling towers). Culturing aerators is relevant for waterborne outbreaks, not for an Aspergillus outbreak linked to renovations, making this option inappropriate.
The best answer is A, culturing the air, as Aspergillus is an airborne pathogen, and renovations are a known risk factor for spore dispersal in healthcare settings. This monitoring strategy allows the infection preventionist to confirm the source, assess the extent of contamination, and implement control measures (e.g., enhanced filtration, construction barriers) to protect patients. This is consistent with CBIC and CDC guidelines for managing fungal outbreaks in high-risk units.
CBIC Infection Prevention and Control (IPC) Core Competency Model (updated 2023), Domain IV: Environment of Care, which recommends air sampling for Aspergillus during construction-related outbreaks.
CBIC Examination Content Outline, Domain III: Prevention and Control of Infectious Diseases, which includes environmental monitoring for facility-acquired infections.
CDC Guidelines for Environmental Infection Control in Healthcare Facilities (2022), which advocate air culturing to detect Aspergillus post-renovation in immunocompromised patient areas.
An infection preventionist reviewing patient records in an outpatient hemodialysis center notes an increase in localized infections at catheter access sites. Which of the following strategies reduces the risk of infection in this population?
Creation of an arteriovenous fistula
Use of a non-cuffed percutaneous catheter
Placement of a femoral catheter
Replacement of dialysis catheters monthly
The best strategy to reduce the risk of infection in hemodialysis patients is to use an arteriovenous (AV) fistula as the preferred vascular access method. AV fistulas have the lowest infection rates compared to catheters and grafts because they do not involve foreign material and are less prone to biofilm formation and bloodstream infections.
Why the Other Options Are Incorrect?
B. Use of a non-cuffed percutaneous catheter – Non-cuffed catheters have a higher risk of bloodstream infections and should be used only for short-term access.
C. Placement of a femoral catheter – Femoral catheters have higher infection risks and should only be used for bed-bound patients and for the shortest duration possible.
D. Replacement of dialysis catheters monthly – Routine catheter replacement does not reduce infection risk and should be done only when medically necessary.
CBIC Infection Control Reference
According to APIC guidelines, AV fistulas are the preferred vascular access due to their lower infection rates and improved long-term outcomes?.
During a COVID outbreak with hospital-associated transmission cases, the infection preventionist (IP) receives a news media call about what is being done to reduce the transmission. The IP's BEST response is to
answer the questions truthfully.
give vague answers to ensure patient privacy.
refer the reporters to the hospital's media spokesperson.
inform the reporter that the conversation must be recorded to ensure accuracy.
The best response for an infection preventionist (IP) when receiving a news media call during a COVID outbreak with hospital-associated transmission cases is to refer the reporters to the hospital's media spokesperson. This approach aligns with the principles outlined in the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, which emphasize the importance of maintaining professionalism, protecting patient privacy, and ensuring accurate communication. The IP's primary role is to focus on infection prevention and control activities rather than serving as a public relations representative. Engaging directly with the media can risk divulging sensitive patient information or operational details that may not be fully contextualized, potentially violating the Health Insurance Portability and Accountability Act (HIPAA) or other privacy regulations.
Option A (answer the questions truthfully) is not ideal because, while truthfulness is important, the IP may not have the authority or full context to provide a comprehensive and accurate public statement, and doing so could inadvertently compromise patient confidentiality or misrepresent hospital policies. Option B (give vague answers to ensure patient privacy) might protect privacy but could lead to miscommunication or lack of trust if the responses appear evasive without a clear referral process. Option D (inform the reporter that the conversation must be recorded to ensure accuracy) is a procedural step but does not address the core issue of who should handle media inquiries.
Referring to the hospital's media spokesperson (Option C) ensures that a trained individual handles the communication, adhering to CBIC's emphasis on collaboration with organizational leadership and adherence to institutional communication protocols (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.1 - Collaborate with organizational leaders). This also aligns with best practices for managing public health crises, where centralized and coordinated messaging is critical to avoid misinformation.
Which of the following strategies is MOST effective in reducing surgical site infections (SSI) in orthopedic procedures?
Perioperative normothermia maintenance.
Routine intraoperative wound irrigation with povidone-iodine.
Administration of prophylactic antibiotics postoperatively for 48 hours.
Use of sterile adhesive wound dressings for 10 days postoperatively.
Perioperative normothermia maintenance reduces SSI rates by improving immune function and tissue perfusion?.
Routine wound irrigation (B) has no strong evidence supporting SSI prevention.
Prolonged antibiotic use (C) increases antibiotic resistance without added benefit.
Extended use of wound dressings (D) does not reduce SSI rates.
CBIC Infection Control References:
APIC Text, "SSI Prevention in Surgery," Chapter 12?.
What data should be collected and analyzed as part of a syndromic surveillance program?
Number of blood and urine cultures
Number of visits to physical therapy
Number of surgical procedures performed
Number of over-the-counter sales of flu remedies
The Certification Study Guide (6th edition) describes syndromic surveillance as a public health surveillance approach that focuses on the early detection of disease outbreaks by monitoring nonspecific indicators that precede formal diagnosis or laboratory confirmation. Rather than relying on confirmed cases, syndromic surveillance tracks patterns of symptoms, behaviors, or indirect data sources that may signal emerging health threats.
One key example emphasized in the study guide is the monitoring of over-the-counter (OTC) medication sales, such as flu and cold remedies. Increases in OTC sales can indicate a rise in respiratory illness within the community before patients seek medical care or receive laboratory testing. This early signal allows infection preventionists and public health officials to initiate investigations, preparedness measures, and targeted messaging sooner than traditional surveillance methods would allow.
The other options reflect data used in traditional or outcome-based surveillance, not syndromic surveillance. Blood and urine cultures require laboratory confirmation and occur later in the disease process. Physical therapy visits and surgical procedure counts are unrelated to early symptom detection and do not provide timely indicators of infectious disease trends.
CIC exam questions frequently test the distinction between traditional surveillance and syndromic surveillance. Recognizing that syndromic surveillance relies on early, indirect indicators of illness, such as OTC medication sales, is essential for accurate exam performance and effective outbreak preparedness.
An infection preventionist observing the technologist in sterile processing load the washer-disinfector or washer-decontaminator should expect to see them:
Fill the load with mixed items to maximize efficiency.
Put the heaviest items on the top rack of the washer.
Disassemble instruments and open hinged instruments.
Place fresh surgical instruments from the case cart directly onto the rack.
Proper loading of a washer-disinfector is designed to maximize detergent and water contact with all instrument surfaces and internal features. CDC guidance for cleaning and sterilizing practices specifically notes that hinged instruments should be opened fully and items with removable parts should be disassembled (unless the manufacturer provides validated instructions indicating otherwise). This ensures the cleaning solution can reach high-risk areas such as box locks, joints, and crevices, which are common sites for retained soil and bioburden.
The other options describe practices that can compromise cleaning effectiveness and safety. “Filling the load with mixed items to maximize efficiency” (A) risks improper positioning, shadowing, and inadequate exposure of surfaces to spray action and detergent. Placing the heaviest items on the top rack (B) is contrary to common reprocessing guidance, which generally places heavier sets lower to prevent damage and to support effective spray patterns.
Finally, instruments should not be taken “directly from the case cart” onto the rack (D) without appropriate sorting/preparation and following the device manufacturer’s instructions for use (IFU), including opening, disassembly, and correct placement in trays/baskets. The expected best practice during loading is therefore disassemble instruments and open hinged instruments
Following an outbreak of Hepatitis A, the water supply is sampled. A high count of which of the following isolates would indicate that the water was a potential source?
Coliforms
Pseudomonads
Legionella
Acinetobacter
Coliform bacteria are indicators of fecal contamination in water, making them a critical measure of water safety. Hepatitis A is a virus primarily transmitted via the fecal-oral route, often through contaminated food or water.
Step-by-Step Justification:
Fecal Contamination and Hepatitis A:
Hepatitis A virus (HAV) spreads through ingestion of water contaminated with fecal matter. High coliform counts indicate fecal contamination and increase the risk of HAV outbreaks?.
Use of Coliforms as Indicators:
Public health agencies use total coliforms and Escherichia coli (E. coli) as primary indicators of water safety because they signal fecal pollution?.
Waterborne Transmission of Hepatitis A:
Hepatitis A outbreaks have been traced to contaminated drinking water, ice, and improperly treated wastewater. Coliform detection signals a need for immediate action?.
Why Other Options Are Incorrect:
B. Pseudomonads:
Pseudomonads (e.g., Pseudomonas aeruginosa) are environmental bacteria but are not indicators of fecal contamination.
C. Legionella:
Legionella species cause Legionnaires' disease through inhalation of contaminated aerosols, not through fecal-oral transmission.
D. Acinetobacter:
Acinetobacter species are opportunistic pathogens in healthcare settings but are not indicators of waterborne fecal contamination.
CBIC Infection Control References:
APIC Text, "Water Systems and Infection Control Measures"?.
APIC Text, "Hepatitis A Transmission and Waterborne Outbreaks"?.
Which of the following processes would the catheter-associated urinary tract infection (CAUTI) improvement team choose as a process indicator to reduce CAUTI?
Documentation of indication for catheter placement
Rate of catheter-associated urinary tract infections
Reduction of catheter insertions per month
Rate of asymptomatic bacteriuria
A process indicator measures whether staff are reliably performing evidence-based practices that prevent infection (i.e., how well we do what we intend to do). For CAUTI prevention, a core, guideline-supported strategy is to use indwelling urinary catheters only for appropriate indications and remove them as soon as they are no longer needed. Because inappropriate placement is a major driver of unnecessary catheter days (and therefore CAUTI risk), tracking whether the clinical indication is documented at insertion is a practical, auditable process measure that directly reflects adherence to appropriate-use policies. The CDC CAUTI prevention toolkit lists “compliance with documentation of catheter …” as an example of a process measure, aligning with performance measurement approaches recommended for CAUTI prevention.
In contrast, the CAUTI rate (option B) is an outcome measure, not a process measure. “Reduction of catheter insertions per month” (option C) reflects volume/usage trends rather than direct compliance with a specific practice, and “rate of asymptomatic bacteriuria” (option D) is not a recommended target metric for CAUTI prevention and routine screening for ASB is discouraged in CAUTI guidance.
An adult with an incomplete vaccination history presents with an uncontrollable, rapid and violent cough, fever, and runny nose. Healthcare personnel should suspect
Pertussis.
Rhinovirus.
Bronchitis.
Adenovirus.
The correct answer is A, "Pertussis," as healthcare personnel should suspect this condition based on the presented symptoms and the patient’s incomplete vaccination history. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, pertussis, caused by the bacterium Bordetella pertussis, is characterized by an initial phase of mild respiratory symptoms (e.g., runny nose, low-grade fever) followed by a distinctive uncontrollable, rapid, and violent cough, often described as a "whooping" cough. This presentation is particularly concerning in adults with incomplete vaccination histories, as the pertussis vaccine’s immunity (e.g., DTaP or Tdap) wanes over time, increasing susceptibility (CBIC Practice Analysis, 2022, Domain I: Identification of Infectious Disease Processes, Competency 1.1 - Identify infectious disease processes). Pertussis is highly contagious and poses a significant risk in healthcare settings, necessitating prompt suspicion and isolation to prevent transmission.
Option B (rhinovirus) typically causes the common cold with symptoms like runny nose, sore throat, and mild cough, but it lacks the violent, paroxysmal cough characteristic of pertussis. Option C (bronchitis) may involve cough and fever, often due to viral or bacterial infection, but it is not typically associated with the rapid and violent cough pattern or linked to vaccination status in the same way as pertussis. Option D (adenovirus) can cause respiratory symptoms, including cough and fever, but it is more commonly associated with conjunctivitis or pharyngitis and does not feature the hallmark violent cough of pertussis.
The suspicion of pertussis aligns with CBIC’s emphasis on recognizing infectious disease patterns to initiate timely infection control measures, such as droplet precautions and prophylaxis for exposed individuals (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.2 - Implement measures to prevent transmission of infectious agents). Early identification is critical, especially in healthcare settings, to protect vulnerable patients and staff, and the incomplete vaccination history supports this differential diagnosis given pertussis’s vaccine-preventable nature (CDC Pink Book: Pertussis, 2021).
After defining and identifying cases in a possible cluster of infections, an infection preventionist should NEXT establish:
The route of transmission.
An appropriate control group.
A hypothesis that will explain the majority of cases.
Whether observed incidence exceeds expected incidence.
When investigating a possible cluster of infections, an infection preventionist (IP) follows a structured epidemiological approach to identify the cause and implement control measures. The Certification Board of Infection Control and Epidemiology (CBIC) outlines this process within the "Surveillance and Epidemiologic Investigation" domain, which aligns with the Centers for Disease Control and Prevention (CDC) guidelines for outbreak investigation. The steps typically include defining and identifying cases, formulating a hypothesis, testing the hypothesis, and implementing control measures. The question specifies the next step after defining and identifying cases, requiring an evaluation of the logical sequence.
Option C, "A hypothesis that will explain the majority of cases," is the next critical step. After confirming a cluster through case definition and identification (e.g., by time, place, and person), the IP should develop a working hypothesis to explain the observed pattern. This hypothesis might propose a common source (e.g., contaminated equipment), a mode of transmission (e.g., airborne), or a specific population at risk. The CDC’s "Principles of Epidemiology in Public Health Practice" (3rd Edition, 2012) emphasizes that formulating a hypothesis is essential to guide further investigation, such as identifying risk factors or environmental sources. This step allows the IP to focus resources on testing the most plausible explanation before proceeding to detailed analysis or interventions.
Option A, "The route of transmission," is an important element of the investigation but typically follows hypothesis formulation. Determining the route (e.g., contact, droplet, or common vehicle) requires data collection and analysis to test the hypothesis, making it a subsequent step rather than the immediate next action. Option B, "An appropriate control group," is relevant for analytical studies (e.g., case-control studies) to compare exposed versus unexposed individuals, but this is part of hypothesis testing, which occurs after the hypothesis is established. Selecting a control group prematurely, without a hypothesis, lacks direction and efficiency. Option D, "Whether observed incidence exceeds expected incidence," is a preliminary step to define a cluster, often done during case identification using baseline data or statistical thresholds (e.g., exceeding the mean plus two standard deviations). Since the question assumes cases are already defined and identified, this step is complete, and the focus shifts to hypothesis development.
The CBIC Practice Analysis (2022) and CDC guidelines prioritize hypothesis formulation as the logical next step after case identification, enabling a targeted investigation. This approach ensures that the IP can efficiently address the cluster’s cause, making Option C the correct answer.
An infection preventionist will know a patient may have a pseudo-infection with a positive urine culture because the patient reports:
Flank pain
No symptoms
Urinary frequency
Costovertebral pain
The CBIC Certified Infection Control Exam Study Guide (6th edition) clearly distinguishes true infection from pseudo-infection and colonization, particularly when interpreting urine culture results. A pseudo-infection refers to a positive laboratory result that does not represent a true clinical infection and is often associated with asymptomatic bacteriuria, specimen contamination, or improper collection.
When a patient has a positive urine culture but reports no urinary or systemic symptoms, the most accurate interpretation is that the finding represents colonization or a pseudo-infection rather than a true urinary tract infection (UTI). The Study Guide emphasizes that UTIs must meet both microbiologic and clinical criteria. Symptoms such as dysuria, urinary frequency, urgency, suprapubic tenderness, flank pain, or costovertebral angle tenderness are required to support a diagnosis of infection.
Options A, C, and D all describe symptoms consistent with upper or lower urinary tract infection and therefore suggest true infection rather than pseudo-infection. In contrast, the absence of symptoms strongly supports a diagnosis of asymptomatic bacteriuria or pseudo-infection, for which antimicrobial treatment is generally not indicated, except in specific populations (e.g., pregnant patients or those undergoing urologic procedures).
Recognizing pseudo-infection is critical for antimicrobial stewardship, prevention of unnecessary antibiotic use, and accurate infection surveillance—key competencies tested on the CIC® exam.
Respiratory tract flora are BEST characterized by which of the following statements?
The airway is sterile below the larynx
Both the upper and lower airways are sterile throughout
Both the upper and lower airways contain small numbers of organisms
The upper airway is heavily colonized while the lower airway is not
The respiratory tract flora refers to the microbial communities inhabiting the respiratory system, and understanding their distribution is essential for infection prevention and diagnosis. The Certification Board of Infection Control and Epidemiology (CBIC) highlights the importance of microbial ecology in the "Identification of Infectious Disease Processes" domain, which aligns with the Centers for Disease Control and Prevention (CDC) and clinical microbiology principles. The question seeks the best characterization of respiratory tract flora, requiring an evaluation of current scientific understanding.
Option C, "Both the upper and lower airways contain small numbers of organisms," is the most accurate statement. The upper respiratory tract (e.g., nasal passages, pharynx) is naturally colonized by a diverse microbial community, including bacteria like Streptococcus, Staphylococcus, and Corynebacterium, as well as some fungi and viruses, acting as a first line of defense. The lower respiratory tract (e.g., trachea, bronchi, alveoli) was traditionally considered sterile due to mucociliary clearance and immune mechanisms. However, recent advances in molecular techniques (e.g., 16S rRNA sequencing) have revealed a low-biomass microbiome in the healthy lower airway, consisting of small numbers of organisms such as Prevotella and Veillonella, likely introduced via microaspiration from the upper tract. The CDC and studies in journals like the American Journal of Respiratory and Critical Care Medicine (e.g., Dickson et al., 2016) support this view, indicating that both regions contain microbial populations, though the lower airway’s flora is less dense and more tightly regulated.
Option A, "The airway is sterile below the larynx," is outdated. While the lower airway was once thought to be sterile, modern research shows a sparse microbial presence, debunking this as a complete characterization. Option B, "Both the upper and lower airways are sterile throughout," is incorrect. The upper airway is clearly colonized, and the lower airway, though low in microbial load, is not entirely sterile. Option D, "The upper airway is heavily colonized while the lower airway is not," overstates the contrast. The upper airway is indeed heavily colonized, but the lower airway is not sterile; it contains small numbers of organisms rather than being completely free of microbes.
The CBIC Practice Analysis (2022) and CDC guidelines on respiratory infections acknowledge the evolving understanding of respiratory flora, emphasizing that both upper and lower airways host small microbial populations in healthy individuals. Option C best reflects this balanced and evidence-based characterization.
A construction project is completed at a healthcare facility and the construction barriers will be removed. Prior to using the space for patient care, an infection preventionist should recommend:
Sampling for airborne contaminants after construction.
Stocking supply rooms as soon as the rooms are available.
Testing the water for Legionella and other waterborne pathogens.
Inspecting and cleaning ducts if needed and balancing the ventilation system.
The Certification Study Guide (6th edition) emphasizes that restoration of a safe environment of care following construction or renovation is essential before patient occupancy. A primary concern after construction is the potential contamination and disruption of the heating, ventilation, and air conditioning (HVAC) system, which plays a critical role in infection prevention by controlling airflow, pressure relationships, and filtration.
Inspecting and cleaning air ducts as needed—and ensuring that the ventilation system is properly balanced—helps confirm that airflow is functioning as designed, including appropriate air exchanges, pressure differentials, and filtration efficiency. The study guide highlights that construction activities can introduce dust, debris, and microorganisms (including fungal spores) into ductwork, which may subsequently be disseminated into patient care areas if not addressed. Proper HVAC verification is a key component of post-construction clearance following an Infection Control Risk Assessment (ICRA).
The other options are not recommended as routine first steps. Air sampling is not advised because results are difficult to interpret and do not reliably predict infection risk. Stocking supplies before environmental clearance risks contamination of clean items. Routine water testing is not required unless water system disruption or stagnation occurred and is guided by a facility’s water management program rather than construction completion alone.
CIC exam questions frequently test post-construction readiness activities, reinforcing that HVAC inspection, cleaning, and balancing are critical prerequisites for safely reopening patient care spaces.
An infection preventionist is observing the cleaning and disinfection process of semi-critical devices. To ensure these items have been reprocessed meeting the minimum requirements, which of the following is required?
Use of detergents with pH lower than 7
Initial cleaning must begin 24 hours after use
Initial cleaning must begin as soon as possible after use
Soaking in a solution of liquid chemical sterilant between 3 and 12 hours
The Certification Study Guide (6th edition) emphasizes that thorough cleaning is the most critical step in the reprocessing of all reusable medical devices, including semi-critical devices (those that contact mucous membranes or nonintact skin). A foundational requirement is that initial cleaning begins as soon as possible after use. Prompt cleaning prevents organic material—such as blood, secretions, and tissue—from drying on device surfaces and within lumens, which can shield microorganisms and significantly reduce the effectiveness of subsequent disinfection.
The study guide explains that delayed cleaning increases the risk of biofilm formation and makes removal of soil more difficult, potentially compromising patient safety. For this reason, point-of-use pre-cleaning and rapid transport to reprocessing are considered minimum expectations. Cleaning must occur before any high-level disinfection or sterilization; without effective cleaning, even correctly selected disinfectants may fail.
The other options are incorrect or misleading. There is no universal requirement for detergents with pH lower than 7; detergent selection should follow manufacturer instructions. Waiting 24 hours before cleaning is contrary to best practice and increases risk. Soaking devices in liquid chemical sterilants for extended periods does not address the prerequisite of cleaning and may not be appropriate for semi-critical devices unless specified by the manufacturer.
This question reflects a key CIC exam principle: timely cleaning is non-negotiable and is the cornerstone of safe device reprocessing.
Which of the following control measures is MOST effective in preventing transmission of Legionella in healthcare water systems?
Flushing all faucets with hot water for 5 minutes daily.
Maintaining hot water storage temperatures above 140°F (60°C).
Installing carbon filters on all hospital water outlets.
Routine testing for Legionella in hospital water.
Maintaining hot water at 140°F (60°C) prevents Legionella growth and is the most effective control strategy?.
Flushing water (A) alone is not sufficient.
Carbon filters (C) do not remove Legionella.
Routine testing (D) is not always necessary unless an outbreak occurs.
CBIC Infection Control References:
APIC Text, "Waterborne Pathogens and Infection Control," Chapter 9?.
The primary source of organisms that cause surgical silo infections is the
operating room environment.
operating room personnel.
patient's endogenous flora
healthcare personnel's hands.
The primary source of organisms causing surgical site infections (SSIs) is the patient’s own endogenous flora. Bacteria from the skin, mucous membranes, or gastrointestinal tract contaminate the surgical site, leading to infection. Common pathogens include Staphylococcus aureus, coagulase-negative staphylococci, and Enterobacteriaceae.
Why the Other Options Are Incorrect?
A. Operating room environment – While environmental contamination can contribute, it is not the primary source.
B. Operating room personnel – Infection control measures (hand hygiene, gloves, masks) reduce transmission from personnel.
D. Healthcare personnel’s hands – Although hand contamination is a risk, it is secondary to the patient’s endogenous flora.
CBIC Infection Control Reference
According to APIC guidelines, the patient’s own flora is the primary source of SSIs?.
Which of the following anti-infective materials is used on endotracheal tubes, urine catheters, and intravascular catheters?
Silver
Copper
Chromium
Zinc
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies silver as an anti-infective material commonly incorporated into medical devices such as endotracheal tubes, urinary catheters, and intravascular catheters. Silver has broad-spectrum antimicrobial properties against bacteria, fungi, and some viruses. When used as a coating or impregnated material, silver ions disrupt microbial cell membranes, interfere with enzyme systems, and inhibit replication—thereby reducing microbial colonization and biofilm formation on device surfaces.
Device-associated infections often originate from colonization of indwelling devices. Silver-coated or silver-impregnated devices are intended to reduce the risk of healthcare-associated infections by limiting early microbial adherence and growth, particularly during the highest-risk period shortly after device insertion. Examples include silver alloy urinary catheters for CAUTI prevention and silver-coated endotracheal tubes designed to reduce ventilator-associated events.
The other options listed are not used in this context. Copper has antimicrobial properties but is not commonly used in indwelling medical devices. Chromium is used for corrosion resistance in alloys, not for infection prevention. Zinc plays roles in wound care and topical formulations but is not standard for catheter or tube coatings.
For CIC® exam preparation, recognizing silver as the anti-infective material used in multiple indwelling devices is important, as it reflects evidence-based strategies aimed at reducing device-associated infection risk.
==========
The cleaning and disinfection process that is appropriate for a particular surgical instrument depends on
all surgical instruments are cleaned and sterilized in the same manner.
instruments contaminated with blood must be bleach cleaned first.
the device manufacturer's written instructions for use.
the policies of the sterile processing department.
The correct answer is C, "the device manufacturer's written instructions for use," as this is the factor that determines the appropriate cleaning and disinfection process for a particular surgical instrument. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, the reprocessing of surgical instruments must follow the specific instructions provided by the device manufacturer to ensure safety and efficacy. These instructions account for the instrument’s material, design, and intended use, specifying the appropriate cleaning agents, disinfection methods, sterilization techniques, and contact times to prevent damage and ensure the elimination of pathogens (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.3 - Ensure safe reprocessing of medical equipment). This is also mandated by regulatory standards, such as those from the Food and Drug Administration (FDA) and the Association for the Advancement of Medical Instrumentation (AAMI), which require adherence to manufacturer guidelines to maintain device integrity and patient safety.
Option A (all surgical instruments are cleaned and sterilized in the same manner) is incorrect because different instruments have unique characteristics (e.g., materials like stainless steel vs. delicate optics), necessitating tailored reprocessing methods rather than a one-size-fits-all approach. Option B (instruments contaminated with blood must be bleach cleaned first) is a misconception; while blood contamination requires thorough cleaning, bleach is not universally appropriate and may damage certain instruments unless specified by the manufacturer. Option D (the policies of the sterile processing department) may guide internal procedures but must be based on and subordinate to the manufacturer’s instructions to ensure compliance and effectiveness.
The emphasis on manufacturer instructions aligns with CBIC’s focus on evidence-based reprocessing practices to prevent healthcare-associated infections (HAIs) and protect patients (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.5 - Evaluate the environment for infection risks). Deviating from these guidelines can lead to inadequate sterilization or instrument damage, increasing infection risks.
An infection preventionist is asked to recommend a product for disinfection of bronchoscopes. Which of the following agents would be appropriate?
Iodophor
Alcohol
Phenolic
Peracetic acid
The correct answer is D, "Peracetic acid," as this agent is appropriate for the disinfection of bronchoscopes. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, bronchoscopes are semi-critical devices that require high-level disinfection (HLD) to eliminate all microorganisms except high levels of bacterial spores, as they come into contact with mucous membranes but not sterile tissues. Peracetic acid is recognized by the Centers for Disease Control and Prevention (CDC) and the Association for the Advancement of Medical Instrumentation (AAMI) as an effective high-level disinfectant for endoscopes, including bronchoscopes, due to its broad-spectrum antimicrobial activity, rapid action, and compatibility with the delicate materials (e.g., optics and channels) of these devices (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.3 - Ensure safe reprocessing of medical equipment). It is commonly used in automated endoscope reprocessors, ensuring thorough disinfection when combined with proper cleaning and rinsing protocols.
Option A (iodophor) is typically used for intermediate-level disinfection and skin antisepsis, but it is not sufficient for high-level disinfection of bronchoscopes unless specifically formulated and validated for this purpose, which is uncommon. Option B (alcohol) is effective against some pathogens but evaporates quickly, fails to penetrate organic material, and is not recommended for HLD of endoscopes due to potential damage to internal components and inadequate sporicidal activity. Option C (phenolic) is suitable for surface disinfection but lacks the efficacy required for high-level disinfection of semi-critical devices like bronchoscopes, as it does not reliably eliminate all microbial threats, including mycobacteria.
The selection of peracetic acid aligns with CBIC’s emphasis on evidence-based reprocessing practices to prevent healthcare-associated infections (HAIs) associated with endoscope use (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.4 - Implement environmental cleaning and disinfection protocols). This choice ensures patient safety by adhering to manufacturer and regulatory guidelines, such as those in AAMI ST91 (AAMI ST91:2015, Flexible and semi-rigid endoscope processing in health care facilities).
The infection preventionist understands that the heating, ventilation and air conditioning (HVAC) systems in the facility can be a risk factor for healthcare-acquired infections. What is the MOST likely risk from the HVAC system for patients in a Pediatric Oncology unit?
Methicillin-resistant Staphylococcus aureus (MRSA)
Norovirus
Aspergillus spp.
Clostridioides difficile
Patients in pediatric oncology units are highly immunocompromised, making them particularly susceptible to opportunistic fungal infections such as Aspergillus spp. HVAC systems, especially if improperly maintained or contaminated, can disseminate fungal spores into patient care areas.
According to the APIC Text (Chapter 116 – HVAC Systems), fungal spores such as Aspergillus can be transmitted via HVAC systems. These infections have been linked to contaminated air ducts, faulty air filters, and construction-related air disturbances. Outbreaks of aspergillosis are frequently associated with construction near patient care areas and are particularly dangerous for immunocompromised patients, including pediatric oncology patients.
Additional data from APIC Text (Chapter 45 – Infection Prevention in Oncology Patients) reinforces that Aspergillus spp. infections in oncology and immunocompromised patients are primarily airborne and are most often disseminated via HVAC systems.
Incorrect answer rationale:
A. MRSA – Typically spread via direct contact, not HVAC.
B. Norovirus – Spread via fecal-oral route and contaminated surfaces, not airborne HVAC.
D. Clostridioides difficile – Spread via contact with spores on surfaces, not through the air.
An infection preventionist has decided to perform surveillance for central line–associated bloodstream infections (CLABSIs) in the facility’s ICU. Which of the following is the MOST appropriate denominator to calculate risk-adjusted rates?
Total number of ICU patients
Total number of patients with central lines
Number of patients with infections who have central lines
Number of days patients have central lines in place
The Certification Study Guide (6th edition) emphasizes that device-associated infection rates must be calculated using time-at-risk denominators to accurately reflect patient exposure. For CLABSI surveillance, the most appropriate denominator is central line days, defined as the total number of days patients have one or more central lines in place during the surveillance period.
Using central line days accounts for both the presence and duration of exposure, which is critical for risk adjustment. The longer a central line remains in place, the greater the opportunity for microbial entry and bloodstream infection. This denominator allows for valid trend analysis over time and meaningful benchmarking with national surveillance systems that use standardized definitions and denominators.
The other options are incorrect because they fail to measure exposure accurately. Total ICU patients and total patients with central lines do not account for how long the device was present. Counting only patients who developed infections incorrectly places outcomes in the denominator, which invalidates rate calculations.
The study guide reinforces that numerators represent infection events, while denominators represent populations or time at risk. For CLABSI, the standard rate is expressed as infections per 1,000 central line days, a core concept frequently tested on the CIC exam.
Accurate denominator selection ensures valid surveillance, supports quality improvement efforts, and enables comparison with national benchmarks—making central line days the correct and most appropriate choice.
A 36-year-old female presents to the Emergency Department with a petechial rash, meningitis, and cardiac arrest. During the resuscitation, a phlebotomist sustained a needlestick injury. The next day, blood cultures reveal Neisseria meningitidis. The exposure management for the phlebotomist is:
Prophylactic rifampin plus isoniazid.
A tuberculin skin test now and in ten weeks.
Work furlough from day ten to day 21 after exposure.
A review of the phlebotomist’s hepatitis B vaccine status.
The scenario involves a needlestick injury sustained by a phlebotomist during the resuscitation of a patient diagnosed with Neisseria meningitidis infection, characterized by a petechial rash, meningitis, and cardiac arrest. Neisseria meningitidis is a gram-negative diplococcus that can cause meningococcal disease, including meningitis and septicemia, and is transmitted through direct contact with respiratory secretions or, in rare cases, blood exposure. The exposure management for the phlebotomist must align with infection control guidelines, such as those from the Certification Board of Infection Control and Epidemiology (CBIC) and the CDC, to prevent potential infection. Let’s evaluate each option:
A. Prophylactic rifampin plus isoniazid: Prophylactic antibiotics are recommended for close contacts of individuals with meningococcal disease to prevent secondary cases. Rifampin is a standard prophylactic agent for Neisseria meningitidis exposure, typically administered as a 2-day course (e.g., 600 mg every 12 hours for adults). Isoniazid, however, is used for tuberculosis (TB) prophylaxis and is not indicated for meningococcal disease. Combining rifampin with isoniazid is incorrect, as it reflects a confusion with TB management rather than meningococcal exposure. This option is not appropriate.
B. A tuberculin skin test now and in ten weeks: A tuberculin skin test (TST) or interferon-gamma release assay (IGRA) is used to screen for latent tuberculosis infection, with a follow-up test at 8-10 weeks to detect conversion after potential TB exposure. Neisseria meningitidis is not related to TB, and a needlestick injury from a meningococcal patient does not warrant TB testing. This option is irrelevant to the scenario and not the correct exposure management.
C. Work furlough from day ten to day 21 after exposure: Neisseria meningitidis has an incubation period of 2-10 days, with a maximum of about 14 days in rare cases. The CDC and WHO recommend that healthcare workers exposed to meningococcal disease via needlestick or mucosal exposure be monitored for signs of infection (e.g., fever, rash) and, if symptomatic, isolated and treated. Additionally, a work restriction or furlough from day 10 to day 21 after exposure is advised to cover the potential incubation period, especially if prophylaxis is declined or contraindicated. This allows time to observe for symptoms and prevents transmission to vulnerable patients. This is a standard infection control measure and the most appropriate initial management step pending prophylaxis decision.
D. A review of the phlebotomist’s hepatitis B vaccine status: Reviewing hepatitis B vaccine status is a critical step following a needlestick injury, as hepatitis B can be transmitted through blood exposure. However, this applies to bloodborne pathogens (e.g., HBV, HCV, HIV) and is not specific to Neisseria meningitidis, which is primarily a respiratory or mucosal pathogen. While hepatitis B management (e.g., post-exposure prophylaxis with hepatitis B immunoglobulin or vaccine booster) should be addressed as part of a comprehensive needlestick protocol, it is not the first or most relevant priority for meningococcal exposure.
The best answer is C, as the work furlough from day 10 to day 21 after exposure addresses the specific risk of meningococcal disease following a needlestick injury. This aligns with CBIC’s focus on timely intervention and work restriction to prevent transmission in healthcare settings. Prophylactic antibiotics (e.g., rifampin) should also be considered, but the question asks for the exposure management, and furlough is a primary control measure. Hepatitis B and TB considerations are secondary and managed separately.
CBIC Infection Prevention and Control (IPC) Core Competency Model (updated 2023), Domain III: Prevention and Control of Infectious Diseases, which includes protocols for managing exposure to communicable diseases like meningococcal infection.
CBIC Examination Content Outline, Domain IV: Environment of Care, which addresses work restrictions and exposure management.
CDC Guidelines for Meningococcal Disease Prevention and Control (2023), which recommend work furlough and monitoring for exposed healthcare workers.
An outbreak of Candida auris is suspected in the infection preventionist's (IP) facility. The IP's investigation must be conducted in a standard method and communication is critical. Which first step is MOST important?
Conduct environmental cultures
Plan to prevent future outbreaks
Notify facility administration
Perform analytical studies
In an outbreak investigation, the first critical step is to notify facility administration and other key stakeholders. This ensures the rapid mobilization of resources, coordination with infection control teams, and compliance with regulatory reporting requirements.
Why the Other Options Are Incorrect?
A. Conduct environmental cultures – While environmental sampling may be necessary, it is not the first step. The outbreak must first be confirmed and administration alerted.
B. Plan to prevent future outbreaks – Prevention planning happens later after the outbreak has been investigated and controlled.
D. Perform analytical studies – Data analysis occurs after case definition and initial response measures are in place.
CBIC Infection Control Reference
APIC guidelines state that the first step in an outbreak investigation is confirming the outbreak and notifying key stakeholders?.
Which of the following represents a class II surgical wound?
Incisions in which acute, nonpurulent inflammation are seen.
Incisional wounds following nonpenetrating (blunt) trauma.
Incisions involving the biliary tract, appendix, vagina, and oropharynx.
Old traumatic wounds with retained devitalized tissue.
Surgical wounds are classified by the Centers for Disease Control and Prevention (CDC) into four classes based on the degree of contamination and the likelihood of postoperative infection. This classification system, detailed in the CDC’s Guidelines for Prevention of Surgical Site Infections (1999), is a cornerstone of infection prevention and control, aligning with the Certification Board of Infection Control and Epidemiology (CBIC) standards in the "Prevention and Control of Infectious Diseases" domain. The classes are as follows:
Class I (Clean): Uninfected operative wounds with no inflammation, typically closed primarily, and not involving the respiratory, alimentary, genital, or urinary tracts.
Class II (Clean-Contaminated): Operative wounds with controlled entry into a sterile or minimally contaminated tract (e.g., biliary or gastrointestinal), with no significant spillage or infection present.
Class III (Contaminated): Open, fresh wounds with significant spillage (e.g., from a perforated viscus) or major breaks in sterile technique.
Class IV (Dirty-Infected): Old traumatic wounds with retained devitalized tissue or existing clinical infection.
Option A, "Incisions in which acute, nonpurulent inflammation are seen," aligns with a Class II surgical wound. The presence of acute, nonpurulent inflammation suggests a controlled inflammatory response without overt infection, which can occur in clean-contaminated cases where a sterile tract (e.g., during elective gastrointestinal surgery) is entered under controlled conditions. The CDC defines Class II wounds as those involving minor contamination without significant spillage or infection, and nonpurulent inflammation fits this category, often seen in early postoperative monitoring.
Option B, "Incisional wounds following nonpenetrating (blunt) trauma," does not fit the Class II definition. These wounds are typically classified based on the trauma context and are more likely to be considered contaminated (Class III) or dirty (Class IV) if there is tissue damage or delayed treatment, rather than clean-contaminated. Option C, "Incisions involving the biliary tract, appendix, vagina, and oropharynx," describes anatomical sites that, when surgically accessed, often fall into Class II if the procedure is elective and controlled (e.g., cholecystectomy), but the phrasing suggests a general category rather than a specific wound state with inflammation, making it less precise for Class II. Option D, "Old traumatic wounds with retained devitalized tissue," clearly corresponds to Class IV (dirty-infected) due to the presence of necrotic tissue and potential existing infection, which is inconsistent with Class II.
The CBIC Practice Analysis (2022) emphasizes the importance of accurate wound classification for implementing appropriate infection prevention measures, such as antibiotic prophylaxis or sterile technique adjustments. The CDC guidelines further specify that Class II wounds may require tailored interventions based on the observed inflammatory response, supporting Option A as the correct answer. Note that the phrasing in Option A contains a minor grammatical error ("inflammation are seen" should be "inflammation is seen"), but this does not alter the clinical intent or classification.
Which of the following is an example of a syndromic surveillance indicator?
Number of individuals presenting with influenza-like illness in the emergency department each day
Number of individuals presenting with laboratory-confirmed influenza in the emergency department each day
Rate of central line–associated bloodstream infections each quarter
Number of cases of methicillin-resistant Staphylococcus aureus in an intensive care unit each month
The CBIC Certified Infection Control Exam Study Guide (6th edition) describes syndromic surveillance as a surveillance method that focuses on clinical signs, symptoms, or health-seeking behaviors rather than confirmed diagnoses. Its primary purpose is early detection of outbreaks or emerging health threats, often before laboratory confirmation is available.
Option A is the correct example because tracking the number of individuals presenting with influenza-like illness (ILI) relies on symptom patterns such as fever, cough, and sore throat. These data are typically collected in near real time from emergency department chief complaints or triage notes, allowing infection preventionists and public health authorities to identify unusual increases quickly and initiate early response measures.
Option B is not syndromic surveillance because it depends on laboratory-confirmed diagnoses, which are characteristic of traditional, diagnosis-based surveillance. Option C represents device-associated infection surveillance, which is retrospective and outcome-focused. Option D involves laboratory-confirmed antimicrobial-resistant organisms and is also not syndromic.
For CIC® exam preparation, it is important to remember that syndromic surveillance prioritizes speed over diagnostic certainty. By monitoring symptom clusters rather than confirmed cases, it enables earlier recognition of outbreaks such as influenza, gastrointestinal illness, or bioterrorism-related events, making it a critical component of public health preparedness and response.
The infection preventionist recognizes that construction barriers are a key component of the Infection Control Risk Assessment (ICRA). The MOST important factor to consider is that construction barriers should:
Be constructed to withstand normal heating, ventilation, and air conditioning (HVAC) airflow rates.
Provide sealed covers for air intakes and exhausts.
Be able to contain dust or infectious microorganisms generated by the project.
Have walk-off mats that are changed daily.
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that the primary purpose of construction barriers within an Infection Control Risk Assessment (ICRA) is to prevent the dissemination of dust and potentially infectious microorganisms generated during construction, renovation, or maintenance activities. Construction activities can aerosolize fungal spores (such as Aspergillus), bacteria, and other particulate matter that pose a significant risk to immunocompromised patients and other vulnerable populations.
Barriers must therefore be designed and maintained to effectively contain dust and microorganisms at the source, preventing their migration into occupied patient care areas. This containment function is the cornerstone of infection prevention during construction and directly aligns with ICRA goals of risk reduction and patient safety.
While the other options describe supportive or secondary considerations, they are not the most critical factor. Withstanding HVAC airflow (Option A) is important, but it serves the larger goal of containment. Sealing air intakes and exhausts (Option B) is a specific engineering control that may be used as part of containment strategies but does not define the primary purpose of barriers. Walk-off mats (Option D) are useful adjunctive controls but are insufficient alone to prevent airborne transmission of contaminants.
For CIC® exam preparation, it is essential to recognize that containment of dust and infectious agents is the defining function of construction barriers within an ICRA, and all other measures support this central objective.
==========
An employee is presenting to Occupational Health for clearance prior to starting work at a healthcare facility. They have a history of having received the Bacillus Calmette-Guérin (BCG) vaccination. What is the preferred methodology for pre-work clearance?
Referral to tuberculosis (TB) clinic
Initial chest radiograph
Interferon-gamma release assay
Two-step purified protein derivative-based Tuberculin skin test (TST)
The preferred methodology for pre-work clearance in this scenario is the interferon-gamma release assay (IGRA), making option C the correct choice. This conclusion is supported by the guidelines from the Certification Board of Infection Control and Epidemiology (CBIC), which align with recommendations from the Centers for Disease Control and Prevention (CDC) for tuberculosis (TB) screening in healthcare workers. The employee’s history of receiving the Bacillus Calmette-Guérin (BCG) vaccination, a vaccine commonly used in some countries to prevent severe forms of TB, is significant because it can cause false-positive results in the traditional Tuberculin skin test (TST) due to cross-reactivity with BCG antigens (CBIC Practice Analysis, 2022, Domain I: Identification of Infectious Disease Processes, Competency 1.3 - Apply principles of epidemiology).
The IGRA, such as the QuantiFERON-TB Gold test, measures the release of interferon-gamma from T-cells in response to specific TB antigens (e.g., ESAT-6 and CFP-10) that are not present in BCG or most non-tuberculous mycobacteria. This makes it a more specific and reliable test for detecting latent TB infection (LTBI) in individuals with a history of BCG vaccination, avoiding the false positives associated with the TST. The CDC recommends IGRA over TST for BCG-vaccinated individuals when screening for TB prior to healthcare employment (CDC Guidelines for Preventing Transmission of Mycobacterium tuberculosis, 2005, updated 2019).
Option A (referral to tuberculosis clinic) is a general action but not a specific methodology for clearance; it may follow testing if results indicate further evaluation is needed. Option B (initial chest radiograph) is used to detect active TB disease rather than latent infection and is not a primary screening method for pre-work clearance, though it may be indicated if IGRA results are positive. Option D (two-step purified protein derivative-based Tuberculin skin test) is less preferred because the BCG vaccination can lead to persistent cross-reactivity, reducing its specificity and reliability in this context. The two-step TST is typically used to establish a baseline in unvaccinated individuals with potential prior exposure, but it is not ideal for BCG-vaccinated individuals.
The IP’s role includes ensuring accurate TB screening to protect both the employee and patients, aligning with CBIC’s focus on preventing transmission of infectious diseases in healthcare settings (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.2 - Implement measures to prevent transmission of infectious agents).
A hospital experiencing an increase in catheter-associated urinary tract infections (CAUTI) implements a quality improvement initiative. Which of the following interventions is MOST effective in reducing CAUTI rates?
Routine urine cultures for all catheterized patients every 48 hours.
Implementing nurse-driven protocols for early catheter removal.
Replacing indwelling urinary catheters with condom catheters for all male patients.
Using antibiotic-coated catheters in all ICU patients.
Nurse-driven catheter removal protocols have been shown to significantly reduce CAUTI rates by minimizing unnecessary catheter use?.
Routine urine cultures (A) lead to overtreatment of asymptomatic bacteriuria.
Condom catheters (C) are helpful in certain cases but are not universally effective.
Antibiotic-coated catheters (D) have mixed evidence regarding their effectiveness?.
CBIC Infection Control References:
APIC Text, "CAUTI Prevention Strategies," Chapter 10?.
There are four cases of ventilator-associated pneumonia in a surgical intensive care unit with a total of 200 ventilator days and a census of 12 patients. Which of the following BEST expresses how this should be reported?
Ventilator-associated pneumonia rate of 2%
20 ventilator-associated pneumonia cases/1000 ventilator days
Postoperative pneumonia rate of 6% in SICU patients
More information is needed regarding ventilator days per patient
The standard way to report ventilator-associated pneumonia (VAP) rates is:

Why the Other Options Are Incorrect?
A. Ventilator-associated pneumonia rate of 2% – This does not use the correct denominator (ventilator days).
C. Postoperative pneumonia rate of 6% in SICU patients – Not relevant, as the data focuses on VAP, not postoperative pneumonia.
D. More information is needed regarding ventilator days per patient – The total ventilator days are already provided, so no additional data is required.
CBIC Infection Control Reference
APIC and NHSN recommend reporting VAP rates as cases per 1,000 ventilator days?.
Major construction and renovations are planned for a hospital’s operating suite, and a meeting is scheduled to plan for construction activities. Aside from the infection preventionist, and representatives from environmental services and engineering, who else should be included in these planning conversations?
Operating room nurse manager
Chief operating officer
Plumbing supervisor
Director of public relations
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that multidisciplinary collaboration is essential when planning construction or renovation projects in patient care areas, especially high-risk locations such as operating suites. In addition to infection prevention, environmental services, and engineering, the operating room nurse manager must be actively involved in construction planning discussions.
The operating room nurse manager represents frontline clinical operations and has direct knowledge of surgical workflows, patient movement, sterile processing needs, case scheduling, and staff practices. Their involvement ensures that construction activities are coordinated to minimize disruption to patient care, maintain sterile environments, and reduce infection risks associated with dust, airflow changes, and traffic patterns. The nurse manager also plays a key role in communicating construction-related precautions and practice changes to surgical staff.
While senior leadership (Option B) may provide oversight, they are not typically involved in detailed infection control planning. The plumbing supervisor (Option C) may be consulted for specific infrastructure issues but does not represent clinical operations. The director of public relations (Option D) is not relevant to construction-related infection risk planning.
The Study Guide highlights that ICRA planning must include clinical leadership from affected areas to ensure that infection prevention measures are practical, effective, and consistently implemented. Including the operating room nurse manager is therefore essential for safe construction planning and is a frequently tested CIC® exam concept.
==========
Based on the Spaulding classification, which of the following pairings is an example of a semi-critical item and its minimal level of disinfection?
Bedside table; high-level disinfection
Surgical instrument; sterilization
Endocavity probe; high-level disinfection
Bedpan; intermediate-level disinfection
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes the importance of applying Spaulding’s classification to determine the appropriate minimum level of processing for medical devices. Under this system, devices are categorized as critical, semi-critical, or noncritical based on the degree of infection risk associated with their use.
Semi-critical items are those that come into contact with mucous membranes or non-intact skin but do not ordinarily penetrate sterile tissue. Examples include endocavity probes, such as transvaginal or transrectal ultrasound probes. Because mucous membranes are more susceptible to infection than intact skin, semi-critical items require at least high-level disinfection after thorough cleaning to eliminate all microorganisms except large numbers of bacterial spores.
Option C correctly pairs an endocavity probe with high-level disinfection, which is the minimum acceptable level of processing for this classification. Option A is incorrect because a bedside table is a noncritical item and requires only low-level disinfection. Option B describes a critical item, which correctly requires sterilization but does not meet the question’s focus on semi-critical devices. Option D is incorrect because bedpans are noncritical items, and intermediate-level disinfection exceeds the minimum requirement.
Understanding Spaulding’s classification and matching devices to the correct level of disinfection is a high-yield topic on the CIC® exam and essential for safe infection prevention practice.
==========
An infection preventionist is preparing a report about an outbreak of scabies in a long-term care facility. How would this information be displayed in an epidemic curve?
List case names, room numbers, and date the infestation was identified using a logarithmic scale.
List case medical record numbers and the number of days in the facility to date of onset, showing data in a scatter plot.
Prepare a bar graph with no patient identifiers showing the number of cases over a specific period of time.
Prepare a scatter plot by patient location showing case prevalence over a specific period of time.
An epidemic curve, commonly used in infection prevention and control to visualize the progression of an outbreak, is a graphical representation of the number of cases over time. According to the principles outlined by the Certification Board of Infection Control and Epidemiology (CBIC), an epidemic curve is most effectively displayed using a bar graph or histogram that tracks the number of new cases by date or time interval (e.g., daily, weekly) without revealing patient identifiers, ensuring compliance with privacy regulations such as HIPAA. Option C aligns with this standard practice, as it specifies preparing a bar graph with no patient identifiers, focusing solely on the number of cases over a specific period. This allows infection preventionists to identify patterns, such as the peak of the outbreak or potential sources of transmission, while maintaining confidentiality.
Option A is incorrect because listing case names and room numbers with a logarithmic scale violates patient privacy and is not a standard method for constructing an epidemic curve. Logarithmic scales are typically used for data with a wide range of values, but they are not the preferred format for epidemic curves, which prioritize clarity over time. Option B is also incorrect, as using medical record numbers and scatter plots to show days in the facility to onset does not align with the definition of an epidemic curve, which focuses on case counts over time rather than individual patient timelines or scatter plot formats. Option D is inappropriate because a scatter plot by patient location emphasizes spatial distribution rather than the temporal progression central to an epidemic curve. While location data can be useful in outbreak investigations, it is typically analyzed separately from the epidemic curve.
The CBIC emphasizes the importance of epidemic curves in the "Identification of Infectious Disease Processes" domain, where infection preventionists use such tools to monitor and control outbreaks (CBIC Practice Analysis, 2022). Specifically, the use of anonymized data in graphical formats is a best practice to protect patient information while providing actionable insights, as detailed in the CBIC Infection Prevention and Control (IPC) guidelines.
An infection preventionist in the role of educator is teaching risk reduction activities to patients and families. For which of the following groups is the pneumococcal vaccine MOST appropriate?
Asplenic patients
International travelers
Immunocompromised newborns
Patients in behavioral health settings
The pneumococcal vaccine is designed to protect against infections caused by Streptococcus pneumoniae, a bacterium responsible for diseases such as pneumonia, meningitis, and bacteremia. The appropriateness of this vaccine depends on the population's risk profile, particularly their susceptibility to invasive pneumococcal disease (IPD). The Certification Board of Infection Control and Epidemiology (CBIC) highlights the role of infection preventionists as educators in promoting vaccination as a key risk reduction strategy, aligning with the "Education and Training" domain (CBIC Practice Analysis, 2022). The Centers for Disease Control and Prevention (CDC) provides specific guidelines on pneumococcal vaccination, recommending it for individuals at higher risk due to underlying medical conditions or immunologic status.
Option A, asplenic patients, refers to individuals who have had their spleen removed (e.g., due to trauma or disease) or have a nonfunctional spleen (e.g., in sickle cell disease). The spleen plays a critical role in clearing encapsulated bacteria like Streptococcus pneumoniae from the bloodstream. Without a functioning spleen, these patients are at significantly increased risk of overwhelming post-splenectomy infection (OPSI), with pneumococcal disease being a leading cause. The CDC and Advisory Committee on Immunization Practices (ACIP) strongly recommend pneumococcal vaccination, including both PCV15/PCV20 and PPSV23, for asplenic patients, making this group the most appropriate for the vaccine in this context. The infection preventionist should prioritize educating these patients and their families about the vaccine's importance and timing.
Option B, international travelers, may benefit from various vaccines depending on their destination (e.g., yellow fever or typhoid), but pneumococcal vaccination is not routinely recommended unless they have specific risk factors (e.g., asplenia or chronic illness) or are traveling to areas with high pneumococcal disease prevalence. This group is not inherently a priority for pneumococcal vaccination. Option C, immunocompromised newborns, includes infants with congenital immunodeficiencies or other conditions, who may indeed require pneumococcal vaccination as part of their routine immunization schedule (e.g., PCV15 or PCV20 starting at 2 months). However, newborns are generally covered under universal childhood vaccination programs, and the question’s focus on "MOST appropriate" suggests a group with a more specific, elevated risk, which asplenic patients fulfill. Option D, patients in behavioral health settings, may have varied health statuses, but this group is not specifically targeted for pneumococcal vaccination unless they have additional risk factors (e.g., chronic diseases), making it less appropriate than asplenic patients.
The CBIC emphasizes tailoring education to high-risk populations, and the CDC’s Adult and Pediatric Immunization Schedules (2023) identify asplenic individuals as a top priority for pneumococcal vaccination due to their extreme vulnerability. Thus, the infection preventionist should focus on asplenic patients as the group for whom the pneumococcal vaccine is most appropriate.
What domain of educational learning involves growth in feelings or emotions?
Affective
Cognitive
Psychomotor
Perceptive
The CBIC Certified Infection Control Exam Study Guide (6th edition) describes three primary domains of educational learning: cognitive, psychomotor, and affective. The affective domain specifically involves growth in feelings, emotions, attitudes, values, motivation, and professional behaviors. This domain addresses how learners internalize information and how education influences beliefs, attitudes, and commitment to practice change.
In infection prevention and control, the affective domain is particularly important because compliance with practices such as hand hygiene, isolation precautions, and use of personal protective equipment depends not only on knowledge or skill, but also on attitudes and values. Education that targets the affective domain helps foster accountability, ethical responsibility, and sustained behavior change among healthcare personnel.
The cognitive domain (Option B) focuses on knowledge acquisition, comprehension, and critical thinking—such as understanding guidelines or surveillance definitions. The psychomotor domain (Option C) involves physical skills and task performance, such as donning PPE or performing aseptic technique. Option D, perceptive, is not a recognized educational learning domain in standard instructional theory.
For the CIC® exam, it is essential to recognize that affective learning influences attitudes and behaviors, making it a key component of successful infection prevention education and culture change initiatives.
Which of the following intravenous solutions will MOST likely promote the growth of microorganisms?
50% hypertonic glucose
5% dextrose
Synthetic amino acids
10% lipid emulsions
10% lipid emulsions are the most likely to promote microbial growth because they provide an ideal environment for bacterial and fungal proliferation, especially Staphylococcus aureus, Pseudomonas aeruginosa, and Candida species. Lipids support rapid bacterial multiplication due to their high nutrient content.
Why the Other Options Are Incorrect?
A. 50% hypertonic glucose – High glucose concentrations inhibit bacterial growth due to osmotic pressure effects.
B. 5% dextrose – While it can support some bacterial growth, it is less favorable than lipid emulsions.
C. Synthetic amino acids – These solutions do not support microbial growth as well as lipid emulsions.
CBIC Infection Control Reference
APIC guidelines confirm that lipid-based solutions support rapid microbial growth and should be handled with strict aseptic technique?.
An infection preventionist (IP) is tasked with identifying if the Intensive Care Unit’s (ICU) central line–associated bloodstream infection (CLABSI) prevention practices are consistent with current best practices. Which of the following quality improvement tools should the IP construct?
Gap analysis
Root cause analysis
Failure mode and effect analysis (FMEA)
Strengths, weaknesses, opportunities, and threats (SWOT) analysis
The Certification Study Guide (6th edition) clearly distinguishes among quality improvement tools based on their purpose and timing. When the goal is to determine whether current practices align with evidence-based standards or best practices, the most appropriate tool is a gap analysis. A gap analysis systematically compares current state practices—such as ICU CLABSI prevention policies, procedures, and compliance data—with the desired state, which is defined by nationally recognized guidelines and best practices.
The study guide emphasizes that gap analysis is particularly useful for program evaluation, policy review, and baseline assessment before implementing improvements. In this scenario, the IP is not responding to an adverse event, nor is the IP proactively predicting failures, but rather assessing alignment with best practices, which is the core function of a gap analysis.
The other tools serve different purposes. Root cause analysis (RCA) is used after an adverse event (such as a CLABSI) to identify contributing factors. Failure mode and effect analysis (FMEA) is a prospective risk assessment tool used to anticipate where processes might fail. SWOT analysis is a strategic planning tool and is not sufficiently specific for evaluating compliance with infection prevention standards.
Because CIC exam questions frequently test the ability to select the right tool for the right situation, recognizing gap analysis as the appropriate choice in this context is essential.
Which of the following active surveillance screening cultures would be appropriate for carbapenem-resistant Enterobacterales (previously known as carbapenem-resistant Enterobacteriaceae) (CRE)?
Rectal or peri-rectal cultures
Nares or axillary cultures
Abscess or blood cultures
Throat or nasopharyngeal cultures
Carbapenem-resistant Enterobacterales (CRE) colonization is most commonly found in the gastrointestinal (GI) tract. Therefore, rectal or peri-rectal cultures are recommended for active surveillance screening.
Why the Other Options Are Incorrect?
B. Nares or axillary cultures – CRE is not primarily found in the nasal or axillary region; this method is more relevant for detecting MRSA.
C. Abscess or blood cultures – While CRE may be present in clinical infections, these cultures are not used for screening asymptomatic carriers.
D. Throat or nasopharyngeal cultures – CRE does not commonly colonize the upper respiratory tract, so these are not ideal for active screening.
CBIC Infection Control Reference
The CDC and APIC guidelines emphasize rectal or peri-rectal swabbing as the most effective active surveillance method for CRE detection?.
3 Months Free Update
3 Months Free Update
3 Months Free Update

TESTED 24 May 2026
